Blood bottles
Notes
Overview
We give a practical guide to the use of blood bottles in clinical practice.
In modern medicine, most hospitals and GP practices are set up with computer software that automatically prints blood labels following a request. This process automatically assigns a test to a blood bottle and reduces the need to handwrite patient information. The required blood bottle on these labels is differentiated by the coloured top (e.g. lavender or gold).
Occasionally, when the test is specialist or there is ‘computer downtime’ knowledge of the appropriate blood bottle is required, but you can always ask! We outline a practical guide to the use of blood bottles and what actually differentiates them.
Blood bottle characteristics
Each blood bottle can be characterised by:
- Coloured top
- Volume of blood (e.g. 3 mL, 4 mL, 6 mL)
- Additive (e.g. EDTA or lithium heparin)
- Mechanism (e.g. vacutainers)
- Material (e.g. plastic or glass)
Colours
The colours of each bottle (or tube!) are specific to the manufacturer and therefore may differ between hospital trusts and GP practices. This is why you may find a specific test is run in two different coloured bottles between hospital trusts. Despite this, some tests are pretty universal within healthcare (e.g. coagulation in light blue top).
Additives
Additives in blood bottles aim to accelerate blood clotting (clot activator) or prevent blood clotting (anticoagulant) to enable specific tests to be run. Inverting the tube after a blood draw helps to mix the blood with the additive to have its desired effect.
Vacutainers
Blood bottles are usually vacutainer tubes that contain a rubber stopper, which creates a vacuum seal inside. This enables a specific amount of blood to be drawn into the tube.
Order of draw
This refers to the specific order in which blood bottles should be taken according to the coloured top. An order is needed because an additive from one tube can be passed to another after piercing the tube with the vacutainer mechanism. Therefore, it aims to prevent cross-contamination. However, in reality, the order is often random.
Blood bottle summary
This is a nice summary of the more common blood bottles used in clinical practice.
Here, we outline common blood bottles by colour, which are displayed in the order of draw. Remember, coloured bottles may differ by manufacturer meaning different additives and thus tests may be used at different laboratories.
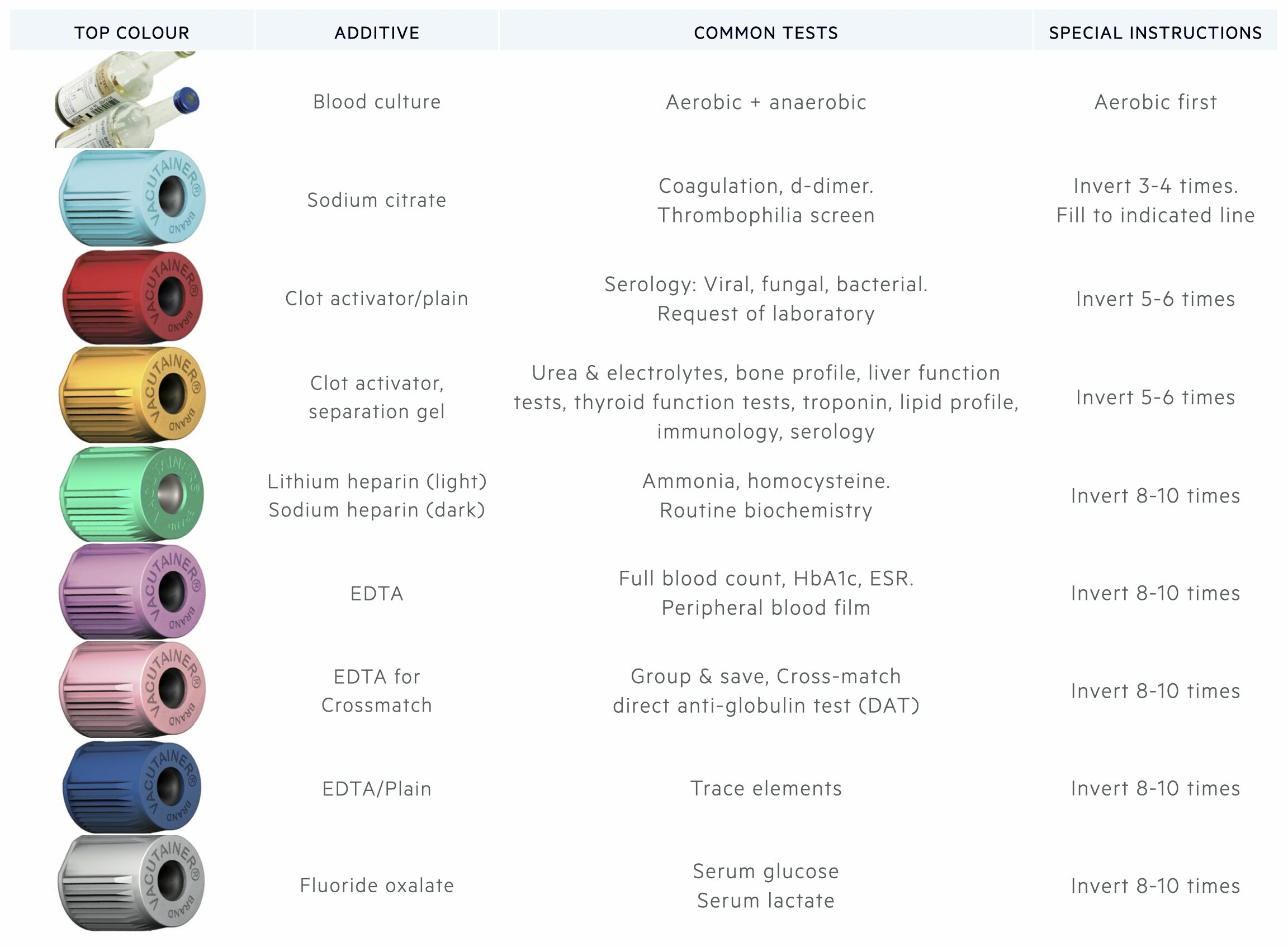
Culture bottles
Bottle cultures are composed of two bottles known as aerobic and anaerobic.
Blood culture bottles have a very classic appearance with specific caps that help indicate the aerobic (e.g. silver/blue top) and anaerobic (e.g. purple top) bottles. Within each bottle is a growth medium to encourage the growth of microorganisms.
As well as phlebotomy, blood culture bottles can be used for small volumes of sterile fluid from other places to aid culture. This may include ascites, synovial fluid, or pleural fluid.
Light blue top
The light blue top is important for assessing coagulation and the clotting system.
The light blue (or just ‘blue’) bottle is important for the assessment of the coagulation system. It contains the additive sodium citrate, which is able to bind to calcium ions that are needed in the clotting cascade. Therefore, binding causes a reversible anticoagulant effect.
This same additive is added to blood transfusion products to prevent clotting. This is why you may get temporary hypocalcaemia following transfusion. Importantly, this blood bottle needs to be filled exactly to the premarked line on the bottle to enable coagulation tests to be run by the lab. A common problem is the test being ‘underfilled’.
Common tests
- International normalised ratio (INR): international standard for PT
- Activated partial thromboplastin time (APTT): assessment of ‘intrinsic’ pathway
- Prothrombin time (PT): assessment of ‘extrinsic’ pathway
- D-dimer
- Activated partial thromboplastin ratio (APTR): to monitor intravenous heparin
Top tip
If you are getting repeated ‘underfilled’ results for coagulation it may be that the vacutainer mechanism is drawing in the initial air from the venepuncture butterfly kit during phlebotomy. In this situation, you may need to use a different blood bottle first.
Red top
The red top is often used for serological tests involving viruses, bacteria, or fungi.
Depending on the manufacturer, the red top may be ‘plain’ meaning it contains no additives or contains a clot activator. It may be used for serological tests involving viruses, bacteria, or fungi. This means looking for specific immunoglobulins (e.g. IgG, IgM) against various microorganisms.
Alternatively, the tube may be requested by the laboratory for very specific tests (e.g. cold agglutinins).
Gold top
The gold (or ‘yellow’) top is used for a wide range of biochemistry tests.
The gold top, also known as the ‘yellow’ top, is one of the most commonly used blood bottles. It is used for a whole variety of biochemistry tests ranging from urea & electrolytes to lipid profiles.
The tube is known as SST (serum separating tube) because it contains two additives that separate the serum from the blood's cellular components. The two additives are silica (a clot activator) and a separation gel that creates the physical barrier between serum and cells. Usually, only a small amount of blood is needed to run tests (good to remember for patients who are ‘difficult to bleed’!). However, a good sample is clearly needed for multiple tests.
Common tests
This list is by no means exhaustive!
- Urea and electrolytes (U&Es): urea, creatinine, sodium, and potassium
- Liver function tests (LFTs): Bilirubin, ALT/AST, ALP, gGT, protein, albumin
- Bone profile: calcium, phosphate, ALP, albumin
- C-reactive protein (CRP)
- Amylase
- Magnesium
- Haematinics: vitamin B12, folate, ferritin
- Iron studies: ferritin, serum iron, transferrin saturation, total iron-binding capacity
- Troponin
- Creatine kinase
- Thyroid function tests (TFTs)
- Immunological & serological tests
Green top
There are two types of green top bottles (dark and light) that differ by their additive.
There are two types of the green top bottles:
- Light green: contains lithium heparin additive (anticoagulant) and a gel separator
- Dark green: contains sodium heparin additive (anticoagulant)
These tubes can be used for the assessment of heparinised blood. The light green tube can be used for plasma, while the dark green tube can be used for plasma or whole blood.
The light green tube may be used as an alternative to the ‘gold top’ to perform routine biochemistry tests and therapeutic drug monitoring. Other commonly performed tests in the green tube are ammonia, TB quantiferon, homocysteine, and more specialist tests (e.g. white cell enzymes).
Lavender top
The lavender (or ‘purple’ top) is mainly used for haematological tests including the standard full blood count.
The lavender (or purple) top is a very commonly used bottle in medicine that contains the additive ethylenediaminetetraacetic acid (EDTA). EDTA binds to calcium within the blood, which has an important role in coagulation, therefore preventing blood from clotting.
The lavender top assesses whole blood and can be used for a range of tests (mainly haematological).
Common tests
- Full blood count
- Haemoglobinopathy screen (e.g. sickle cell anaemia and thalassaemia)
- Reticulocytes
- HbA1c: assess glycated haemoglobin (glucose control over months)
- Glucose-6-phosphate dehydrogenase (G6PD)
- Peripheral blood film
- Malaria parasites
- Drug levels (e.g. tacrolimus/ciclosporin)
- Parathyroid hormone (PTH)
Pink top
The pink top is often known as the ‘group and save’ bottle that is needed to blood group patients and to perform a crossmatch.
The pink top bottles are mainly used by the transfusion lab for analysis of whole blood to enable the allocation of group-specific blood in patients who need a transfusion. The bottle contains EDTA, similar to the lavender top, that acts as an anticoagulant.
Common tests
- Group and save (G&S)
- Crossmatch
- Direct antiglobulin test (DAT): essentially checking for the presence of antibodies attached to red blood cells (may indicate autoimmune haemolytic anaemia).
Understanding transfusion tests
There are two key tests to understand:
- Group and save (or group and screen): determines the patients' blood type (e.g. ABO) and rhesus status (e.g. RhD +ve or -ve). Also enables screening of atypical antibodies (i.e. antibodies that will react to donor blood). This checks the patients' blood but does not issue blood products.
- Crossmatch: physical mixing of a patients' blood (recipient) with the donors' blood. It is a direct compatibility test that checks whether serum containing immunoglobulins from the recipient reacts with red blood antigens from the donor. A full crossmatch takes 40-60 minutes. This needs to be considered if blood is needed more urgently.
NOTE: the rhesus blood group has many proteins, but the most significant is protein D. Thus, being rhesus positive (+ve) or negative (-ve) refers specifically to the presence or absence of the D protein.
Transfusion safety
For transfusion safety, a patient must have two documented group and save samples in the laboratory before a crossmatch is completed. In addition, samples should be taken at least 15 minutes apart (often by two different individuals). Many hospitals will require samples to be handwritten at the bedside checking the patients' identity. Other hospitals may have a computer tracking system that prints labels by scanning the patients' ID at the bedside following identify check.
Appropriate elearning should be provided to all healthcare professionals when joining a new trust with regard to blood transfusion safety.
Royal blue top
The royal blue bottle is rarely used but is needed to check for trace elements.
The royal blue bottle contains the additive EDTA that acts as an anticoagulant. Other types of royal blue bottles may not contain any additive and are referred to as ‘plain’. These bottles check for trace elements including copper, zinc, selenium, iodine and aluminum amongst others. These are often checked in patients having long-term total parenteral nutrition (TPN).
Grey top
The grey top bottle is most commonly used to check serum glucose levels.
The grey top bottle can be used to check for two main tests: serum glucose and serum lactate. Given the widespread use of point of care venous blood gas analysis, the measurement of serum lactate is rarely done. However, it may be needed for checking lactate in different sample types (e.g. cerebrospinal fluid).
The tube contains both sodium fluoride that acts as a preservative to prevent glycolysis and potassium oxalate that acts as an anticoagulant. This is often shortened to fluoride oxalate. The grey top bottle is invaluable in patients presenting with diabetic complications (e.g. diabetic ketoacidosis) when the capillary blood glucose monitor just reads ‘HI’.
Last updated: May 2022
Have comments about these notes? Leave us feedback
