Impetigo
Notes
Overview
Impetigo is a common superficial bacterial skin infection that is highly contagious.
Impetigo is considered the most common bacterial infection in children but can occur at any age. It relates to a superficial infection in the upper layer of the skin, known as the epidermis. The most commonly implicated bacteria as Staphylococcus aureus and Group A Streptococcus. Topical antibiotics are usually sufficient to treat the condition.
Aetiology & pathophysiology
Impetigo is commonly caused by Staphylococcus aureus, which is a gram-positive coccus.
Impetigo is usually caused by microorganisms that are commonly found on the skin. Bacteria are able to enter through breaks in the skin that are caused by minor trauma (e.g. scratching). Here, they can multiple and initiate an infection.
Classification
Impetigo may be divided into primary or secondary.
- Primary: direct bacterial invasion into previously normal skin
- Secondary: infection occurring at a site of skin trauma (e.g. insect bites, eczema, abrasions)
Bacteria
Staphylococcus aureus is commonly implicated in impetigo, which is a gram-positive coccus. There is a growing number of cases related to methicillin-resistant Staphylococcus aureus (MRSA). Other commonly implicated bacteria include Group A Streptococcus and occasionally other groups of Streptococci.
Spread
Impetigo is highly contagious and may be spread easily among close contacts through direct contact. This may occur due to contamination of surrounding objects such as toys or towels.
Several factors increase the risk of spread including pre-existing skin disease, humid/hot weather, poor hygiene, and crowding.
Clinical features
Impetigo classically causes lesions with golden/brown crusting over the face.
There are two clinical presentations, or forms, of impetigo:
- Non-bullous: Majority of cases (~70%). Due to Staphylococcus or Streptococcus.
- Bullous: Minority of cases, evidence of large fluid-filled blisters, usually due to Staphylococcus.
Non-bullous
Small vesicles (fluid-filled cyst < 5 mm) or pustules (pus-filled cyst) develop at the site of infection and then rupture leading to the release of exudate that crusts over with a classic golden/brown colour. The crusts then dry over and separate from the skin leaving a mild area of erythema before healing over 2-3 weeks. Lesions may be itchy, but commonly asymptomatic.
Common sites:
- Face: perioral and perinasal areas common
- Limbs
- Flexures
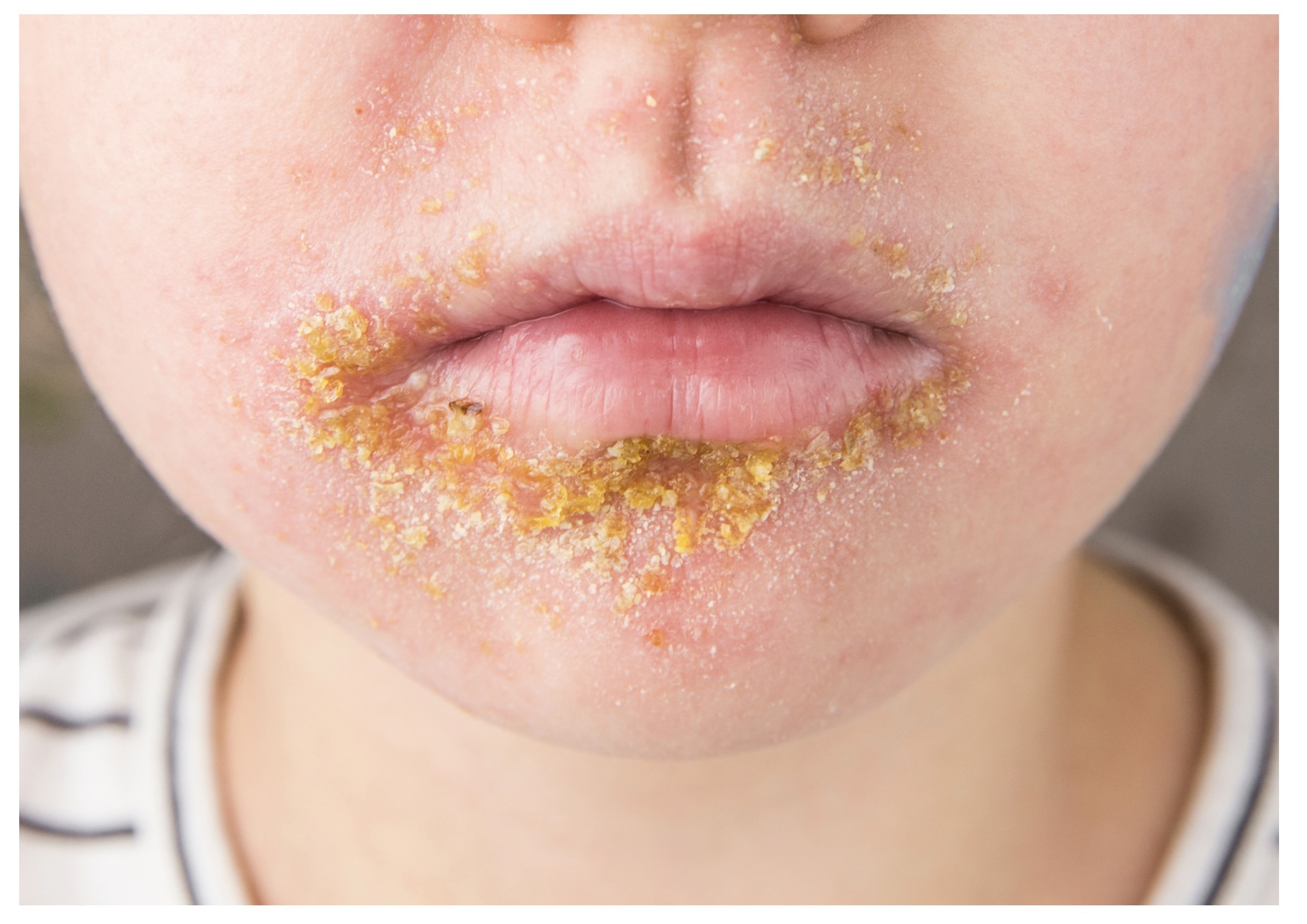
Impetigo affecting the perioral region in a child
Bullous
Bullous impetigo is characterised by the development of large bullae (fluid-filled cysts > 5 mm) that may increase to 2 cm in size and then rupture leaving a thin yellow/brown crust. Similar to non-bullous impetigo, these lesions dry up and heal over 2-3 weeks. Patients may have systemic features (fever, lethargy, diarrhoea) if large areas are affected.
Common sites:
- Flexures
- Face
- Limbs
- Trunk
Diagnosis & investigations
Impetigo is commonly a clinical diagnosis based on the characteristic appearance.
Impetigo is a clinical diagnosis based on the characteristic appearance of golden/brown crusting over typical areas such as the face. There may be evidence of background skin changes due to an underlying condition such as eczema.
If in doubt, the diagnosis can be confirmed with skin swabs for microscopy, culture, and sensitivity.
Management
Topical antibiotics are usually the treatment of choice in impetigo.
Patients and parents should be advised that lesions will heal without scarring and should maintain good hygiene measures to reduce transmission. Children and adults should not attend school/nursery or work until lesions have at least crusted over or after 48 hours of antibiotics.
Medical treatment options depend on the type of impetigo and can include both topical and oral treatments. If symptoms do not improve with initial treatment, then an alternative regimen should be used and consideration for undertaking microbiological testing (e.g. skin swab) and MRSA screening.
Localised non-bullous
For uncomplicated cases, treatment may include the 5 days of the following:
- Hydrogen peroxide 1% cream
- Fusidic acid 2% (5 days)
- Mupirocin 2% (5 days)
Treatment can be extended to 7 days and a microbiologist should be consulted if MRSA is suspected or confirmed.
Widespread non-bullous
For more extensive non-bullous disease, topical or oral antibiotics may be offered for a total of 5 days.
- Topical fusidic acid 2%
- Topical Mupirocin 2%
- Oral flucloxacillin
- Oral macrolide (e.g. erythromycin/clarithromycin): if penicillin-allergic
Again, the length of treatment can be extended to 7 days but importantly topical and oral therapy should not be combined.
Bullous
Any patient with bullous impetigo, or who is systemically unwell, should be offered a course of oral antibiotics.
- Oral flucloxacillin
- Oral macrolide (e.g. erythromycin/clarithromycin): if penicillin-allergic
The length of treatment can be extended to 7 days. If symptoms worsen then the patient may need admission to hospital (see severe disease).
Severe disease
Patients with rapidly developing symptoms, systemically unwell, or have severe complications may require admission to the hospital for intravenous antibiotics and further management.
Complications
The majority of infections are mild and easily treatable.
Impetigo is usually an easily treated infection and the majority of patients will get better with no complications. Complications can include:
- Acute glomerulonephritis (following streptococcal impetigo): most commonly occurs 1-2 weeks after infection
- Cellulitis: deeper infection affecting the dermis and subcutaneous tissue
- Staphylococcal scalded skin syndrome: due to release of an exotoxin that causes severe damage to the epidermis from toxigenic strains of S. Aureus
- Lymphangitis: infection of the lymphatic system
- Osteomyelitis and septic arthritis
- Scarlet fever (following streptococcal infection): diffuse erythematous eruption due to delayed hypersensitivity to a group A streptococcus exotoxin
Last updated: September 2021
Have comments about these notes? Leave us feedback