Psoriasis
Notes
Introduction
Psoriasis is a common, chronic, inflammatory papulosquamous disorder typically characterised by well-demarcated, scaly plaques and a relapsing-remitting course.
Psoriasis is a common skin disorder that affects an estimated 1-3% of the world's population. There are a number of distinct clinical patterns, the most common being chronic plaque psoriasis which accounts for 80-90% of cases.
It is frequently associated with systemic diseases (e.g. psoriatic arthritis) and can also impact individuals' self-esteem and mental wellbeing. Treatment tends to be with topical therapies (e.g. emollients, steroids, vitamin D analogues) with phototherapy and systemic therapies reserved for more severe or treatment-resistant disease.
Epidemiology
The majority of patients with psoriasis will present before the age of 35 years old.
Globally, psoriasis is a common condition and the prevelance is estimated at 1.92% (95% confidence intervals: 1.07-3.46%) in Western Europe.
A higher prevalence of psoriasis has been reported in white people when compared to other ethnicities. Overall there is an equal gender balance.
Risk factors
There are a number of factors that may trigger or exacerbate disease.
- Genetics: there appears to be a strong genetic component to psoriasis. Genome-wide association studies have identified a number of loci that seem related to its development. This includes the Major Histocompatibility Complex region on chromosome 6.
- Streptococcal infection: related to guttate psoriasis, a specific form characterised by the sudden eruption of small circular plaques following a ‘strep throat’ infection.
- Trauma: in some patients, trauma to the skin can trigger psoriasis in an area that was previously unaffected. This is an example of the Koebner phenomenon where new lesions of a pre-existing dermatosis occur at sites of skin trauma.
- Hormones: changes in disease activity are seen with changes in levels of various hormones. Disease is often worse during puberty, menopause and the postpartum period. During pregnancy, many patients see an improvement in their psoriasis but a minority have a worsening.
- Drugs: a number of medications have been shown to worsen disease or result in psoriasis-like drug reactions. These include beta-blockers, lithium, chloroquine and ACE inhibitors. The withdrawal of steroids may precipitate a rebound or the development of erythrodermic or generalised pustular disease.
Other risk factors include:
- HIV
- Smoking
- Alcohol
- Stress
Pathophysiology
Psoriasis is an immune-mediated disease featuring hyperproliferation of the epidermis.
The pathophysiology of psoriasis is complex and incompletely understood. It has been demonstrated that the immune system plays a key role - becoming activated and resulting in inflammatory plaques on the skin.
It is thought that antigenic stimuli initiate an immune response from elements of the innate immune system in the skin of susceptible individuals. This results in the release of inflammatory mediators (e.g. interferon-alpha). Myeloid dendritic cells are attracted and activated producing interleukin-23 triggering the involvement of T cells. Further cytokine production (including interleukin-17A) amongst other factors stimulate hyperproliferation of keratinocytes.
Associated conditions
It is estimated that a third of patients with psoriasis will develop psoriatic arthritis.
Psoriatic arthritis
Psoriatic arthritis is a chronic seronegative inflammatory arthritis. It is estimated that around a third of people with psoriasis will develop psoriatic arthritis (though figures vary). The onset of arthritis normally follows that of skin disease by 5-10 years though occasionally this temporal relationship is reversed.
Psoriatic nail disease affects 90% of patients with a combination of psoriasis and psoriatic arthritis.
Other conditions
There are a number of other conditions that are associated with psoriasis. Patients are more likely to have inflammatory bowel disease (in particular Crohn’s disease), metabolic syndrome, cardiovascular disease and other autoimmune disorders.
Several ocular pathologies appear to occur with greater frequency including uveitis, blepharitis and conjunctivitis.
Subtypes
Psoriasis is a complex skin condition with a number of clinical subtypes, the most common being chronic plaque psoriasis which accounts for 80-90% of cases.
Chronic plaque psoriasis
Chronic plaque psoriasis is the most common subtype and is characterised by raised, scaly, well-demarcated plaques. It is typically symmetrically distributed and often affects the scalp, extensor surfaces, trunk, gluteal cleft and knees. Lesions are typically itchy and may become fissured and painful over joint lines, on the palms of the hand or soles of the feet.
The appearance of psoriasis may differ depending on skin colour. In fair-skinned populations, plaques are typically described as erythematous and pink or red with a silver-white scale. In Hispanics the plaques may be salmon coloured with a silver-white scale. On black skin, psoriasis may have a somewhat violet appearance with a scale that appears more greyish. On more pigmented skin post-inflammatory hyperpigmentation may occur.
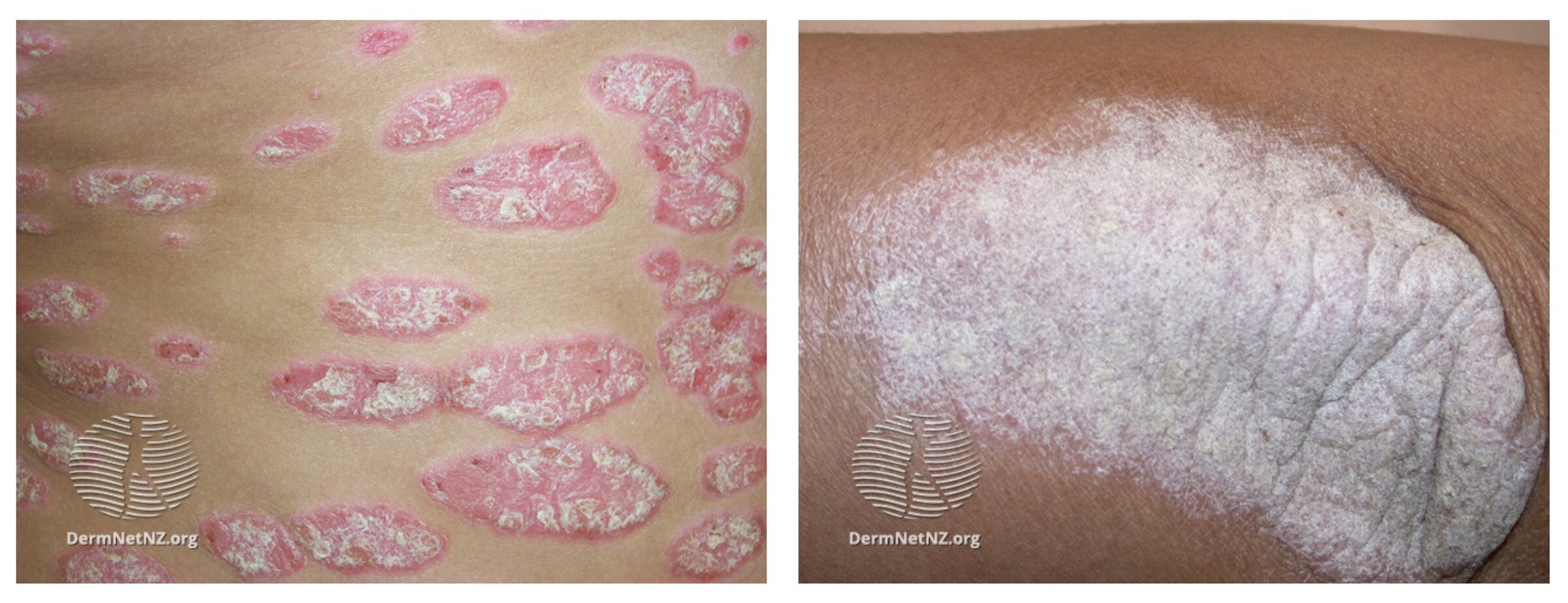
Chronic plaque psoriasis
Image courtesy of DermNet NZ, Creative Commons licence
Nail psoriasis
Nail changes can be seen in patients with all subtypes of psoriasis. Fingernails are involved in around 50% of cases and toenails in 35%. In patients with psoriatic arthritis, nail changes are very common affecting 90%.
Typical changes include:
- Subungual hyperkeratosis
- Nail pitting
- Oil drop discolouration (yellow/pink patches)
- Leukonychia (white discolouration)
- Onycholysis (detachment of the nail from the nail bed)
- Splinter haemorrhages
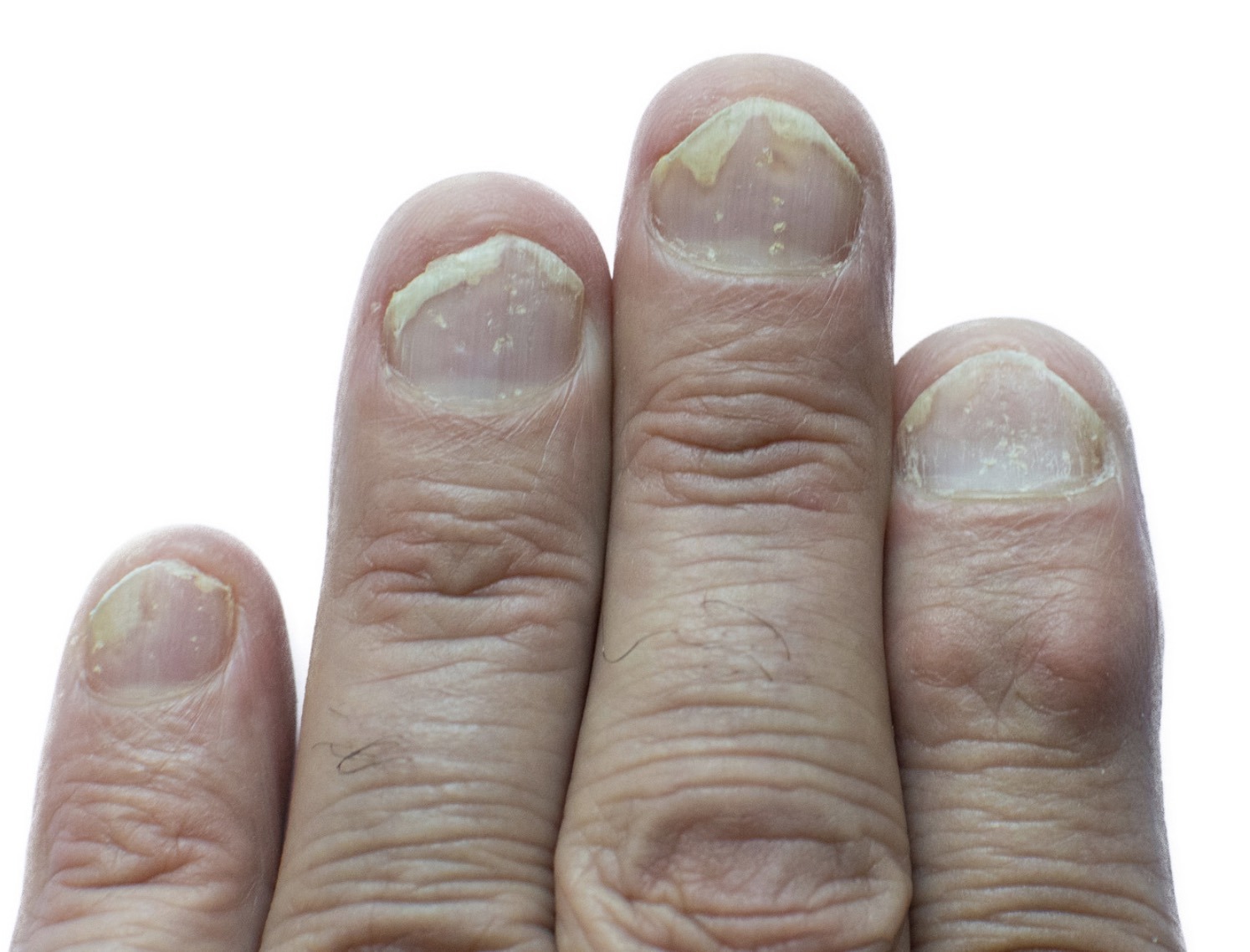
Nail psoriasis
Inverse psoriasis
Also termed flexural psoriasis, inverse psoriasis follows a different pattern of distribution to chronic plaque psoriasis. It affects ‘Intertriginous’ areas - points where skin touches/rubs together. Areas affected include the axilla, groin and genital area, inframammary folds and gluteal cleft.
Guttate psoriasis
Also termed raindrop psoriasis, it presents as a sudden eruption of small circular plaques classically 2 weeks following a streptococcal sore throat. It can also occur as a flare of disease in patients with pre-existing psoriasis.
It is generally self-limiting resolving over 3-4 weeks but around a third will develop classic plaque psoriasis.
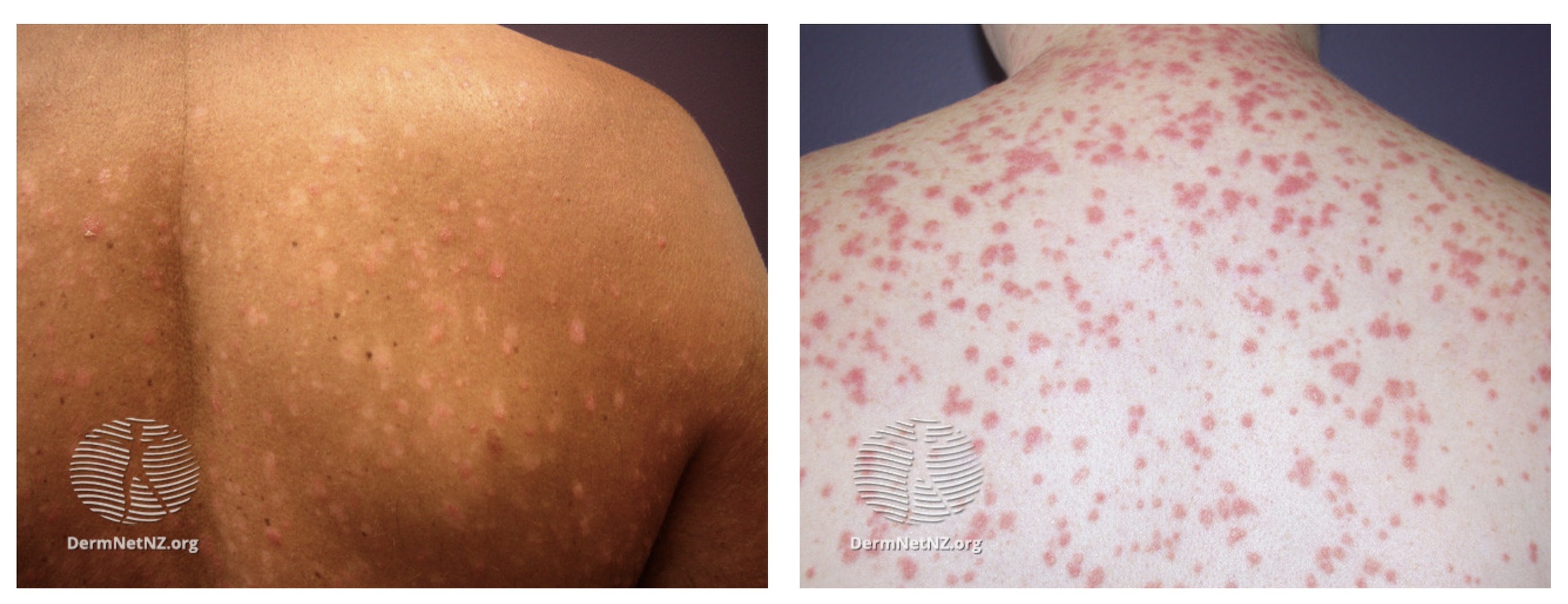
Guttate psoriasis
Image courtesy of DermNet, Creative Commons licence
Erythrodermic psoriasis
Erythrodermic psoriasis is a rare subtype accounting for around 1-2.5% of cases. It refers to a severe form of the disease characterised by widespread erythema and psoriasis affecting a large portion of the bodies surface area (at least 75-90%). It often occurs on the background of known psoriasis but may represent the first presentation.
Triggers include recent illness (particularly infectious), medications (e.g. steroids) and emotional stress. It presents with a range of severity but can be life-threatening. Patients require hospitalisation (in most cases), supportive care and specialist management. Immunosuppressive agents and biologics (e.g. infliximab) are used in its treatment.
Generalised pustular psoriasis
Generalised pustular psoriasis (GPP) can be subdivided into acute GPP and generalised annular pustular psoriasis. Acute GPP is characterised by rapidly developing and widespread erythema and pustules. The pustules may coalesce forming ‘lakes of pus’. They tend to resolve over days leaving the erythema and scaring. It can represent a dermatological emergency and patients are often systemically unwell with fever, malaise and arthralgia.
Generalised annular pustular psoriasis follows a subacute, recurring course. Patients develop plaques with peripheral pustules.
Localised pustular psoriasis
Localised (palmoplantar) psoriasis generally affects the hand and feet. Pustules develop along with plaques. It is strongly associated with smoking.
Management
The management of chronic plaque psoriasis may involve topical agents, phototherapy and systemic therapies.
Psoriasis is (in most cases) a chronic condition and though no cure exists, treatments can be effective at reducing and even clearing disease. It can be expected to recur, particularly after the cessation of treatment.
There are a number of sub-types of psoriasis each with its own treatment pathway. Here we will focus on the most common form, chronic plaques psoriasis.
Topical agents are typically offered first line. Phototherapy and systemic therapies are generally used second or third line but maybe initiated earlier in those with severe/extensive disease or where topical agents are ineffective (e.g. nail disease).
Topical therapies
Topical therapies help to reduce both symptoms (itch) and reduce/clear plaques. Active agents such as topical steroids and vitamin D analogues are added to regular emollient use.
The choice of agent should take into account patient factors, preferences, side effect profiles and the practicality of the various regimens. Options include:
- Emollients: these are moisturising agents that help to reduce itching and remove scaling. They can be used liberally and regularly.
- Topical steroids (e.g. beclometasone): have an anti-inflammatory effect and may be used for limited defined courses. A range of strengths are available and to correct form must be chosen depending on the site of disease. Mild steroids may be used on the face/skin folds, with stronger formulations used on extensor sites. Potent steroids have been linked to the development of erythroderma and generalised pustular psoriasis.
- Vitamin D analogues (e.g. calcipotriol): modulates the immune system and reduces hyperkeratosis. Can be used as a long-term treatment option. Care with dosing is important to avoid hypercalcaemia. Avoided in pregnancy and breastfeeding.
- Vitamin A analogue (tazarotene): typically used sparingly, avoiding the face and skin folds. Irritation is common and limits use. Contraindicated in pregnancy and breastfeeding.
- Tar preparations: helps to reduce scaling and slow plaque formation. It comes in a variety of forms including shampoo, creams and ointments.
- Short contact dithranol: dithranol is used for short periods of time (e.g. 10-30 minutes) before being rinsed off. It can be applied to chronic extensor plaques only, avoiding normal skin. It stains objects it comes into contact with and may temporarily stain skin.
Phototherapy
Phototherapy is used as second or third-line therapy in patients with disease that does not respond adequately to first-line topical measures. Care is guided by dermatologists following a referral from primary care. There are two main forms of phototherapy used to treat psoriasis:
- UVB: narrow-band ultraviolet B therapy may be used in patients with plaque psoriasis that has not adequately responded to topical therapy.
- PUVA: is a form of photochemotherapy which uses a combination of a photosensitising drug and UV therapy. PUVA, used in resistant disease, refers to the combination of psoralen (topical and oral preparations available) with ultraviolet A. Complications include skin irritation, damage and skin cancer (a risk that is compounded if given ciclosporin).
Systemic treatments
Systemic therapies efficacy has to be weighed against their potentially severe side effects. As such their use is controlled by dermatologists. In those requiring systemic treatment the options include:
- Methotrexate: is an antifolate immunosuppressant normally used first-line in patients requiring systemic therapy. It reduces the hyperproliferation of keratinocytes. It is teratogenic and cannot be used in pregnancy or in those breastfeeding. Contraception is advised for both men and women during, and for at least 6 months after, treatment.
- Ciclosporin: is a calcineurin inhibitor with immunosuppressant action. It is often used where rapid control is needed (e.g. acute flare), in palmoplantar pustulosis and where patients are considering pregnancy and there is no opportunity to avoid systemic therapy.
- Acitretin: is a retinoid. Its use is restricted, generally only for those who have failed other systemic options or in whom they are inappropriate. The MHRA have specific guidance for patients with the potential to get pregnant. Pregnancy must be avoided during therapy and for 3 years after.
- Biologics (e.g. infliximab): biologics like infliximab are monoclonal antibodies that modulate elements of the immune system. They are administered as IV injections and are generally reserved for severe and treatment-resistant disease.
Complications
Psoriasis is associated with an increased risk of psychosocial difficulties.
- Psychological: psoriasis may affect individuals' self-esteem and affect personal relationships. Mental health illnesses like anxiety and depression can occur and should be regularly screened for.
- Systemic upset: erythrodermic psoriasis and generalised pustular psoriasis can lead to significant systemic upset, impaired organ function and may be life-threatening.
- Medication-related: many of the medications used in the treatment of psoriasis have troubling or severe side-effects. These range from skin irritation to teratogenicity to malignancies.
Last updated: April 2022
Have comments about these notes? Leave us feedback
