Urticaria
Notes
Overview
Urticaria is a skin rash characterised by red, raised, itchy areas that result from release of chemical mediators such as histamine.
Urticaria is a common skin rash that may be referred to as ‘hives’ or ‘wheals’. It is characterised by the presence of very itchy (pruritic) erythematous papules. The urticarial lesions may be a few millimetres to several centimetres in size and can coalesce to cover larger areas.
Urticaria is common occurring in 20% of the population during their lifetime. Urticaria may co-exist with angio-oedema and be part of a more generalised allergic reaction (i.e. anaphylaxis).
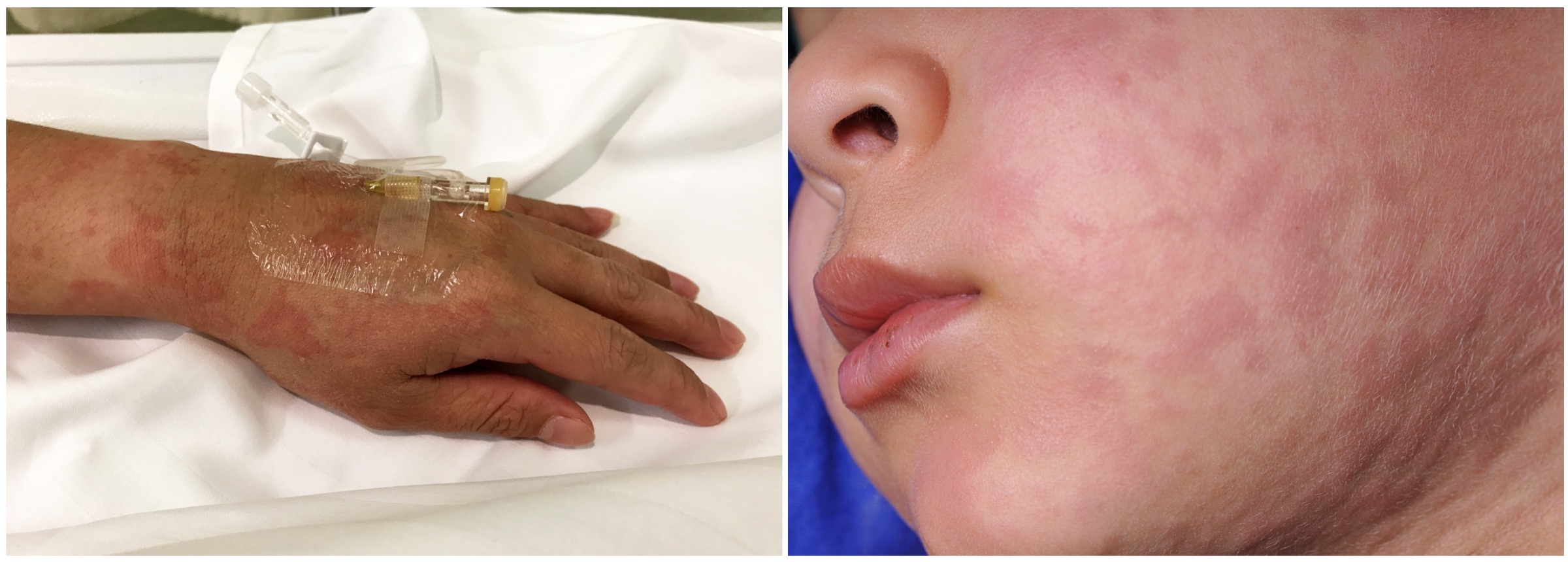
Typical examples of urticaria
Classification
Urticaria may be described as acute or chronic.
Urticaria, with or without angio-oedema, is defined as acute or chronic by an arbitrary time cut-off.
- Acute: urticaria < 6 weeks duration
- Chronic: recurrent urticaria (i.e. most days of the week) > 6 weeks duration
Acute urticaria
Most cases of acute urticaria will resolve within hours to days of onset. There are numerous causes of acute urticaria. In addition, acute urticaria is more likely to have an identifiable cause than chronic urticaria.
Chronic urticaria
Chronic urticaria is broadly divided into ‘inducible’ and ‘spontaneous’.
- Inducible: refers to urticaria being triggered by a physical stimulus (e.g. cold, heat, pressure, water, exercise)
- Spontaneous: recurrent urticaria and/or angio-oedema that is mainly idiopathic (unknown cause). Small number of cases are associated with underlying chronic infection or autoimmune condition.
NOTE: Dermographism refers to an exaggerated skin reaction with formation of urticaria after the skin is stroked or scratched. It is sometimes referred to as ‘skin writing’ and can affect 5% of the population although most patients are otherwise healthy.
Pathophysiology
The hallmark mechanism of urticaria is the release of chemical mediators by mast cells.
Urticaria is due to the release of inflammatory mediators by mast cells and basophils in the upper dermis. Both immune (e.g. IgE-mediated) and non-immune mechanisms can lead to the release of these inflammatory mediators including histamine and cytokines. These cause vasodilatation in the skin leading to localised swelling and marked itching.
Angio-oedema results from vasodilatation and movement of fluid into peripheral tissue in the deep dermis and subcutaneous layer. This characteristically occurs in non-gravitational dependent areas (e.g. face, lips, larynx, bowel). Angio-oedema may result from the release of inflammatory mediators by mast cells similar to urticaria or to the release of bradykinin that affects vascular permeability.
Importantly, bradykinin-mediated angio-oedema is not associated with urticaria and/or pruritus.
Aetiology
There are numerous causes of urticaria but often an underlying aetiology cannot be identified.
The underlying cause of urticaria may be described as IgE-mediated or non-IgE-mediated.
- IgE-mediated: Refers to a type 1 hypersensitivity reaction (i.e. allergic reaction). These reactions occurs within minutes to hours of exposure and may be associated with angio-oedema or anaphylaxis.
- Non-IgE-mediated: A variety of mechanisms may lead to development of urticaria through direct mast cell activation, heightened sensitivity of mast cells to environmental factors or other immunological mechanisms. The majority of urticaria is non-IgE-mediated.
Acute urticaria
Common causes of new-onset urticaria include infections, insect bites or stings, medications and food.
- Infections: may occur following viral or bacterial infections. Very common in children. Parasites such as Echinococcus or Strongyloides may also cause self-limiting urticaria with eosinophilia
- Insect bites & stings: usually IgE-mediated reactions to wasp/bee stings or bedbug/flea bites
- Food allergy: virtually any food can cause an allergic reaction. Some like milk, eggs or peanuts cause an IgE-mediated allergic reaction. Others such as strawberries or tomatoes may cause generalised urticaria or contact urticaria via other mechanisms
- Drug reactions: frequently secondary to antibiotics (e.g. penicillins). Non-IgE-mediated urticaria may occur from opiates, radiological contrast medium, vancomycin or muscle relaxants (e.g. atracurium)
- NSAIDs: may cause urticaria by an allergic (IgE) reaction or non-immunological reactions due to the cyclooxygenase 1 (COX-1) inhibiting properties of certain NSAIDs. These non-immunological reactions are often termed ‘pseudoallergies’ and divided into types
- Contact with allergens: physical contact with certain substances can produce urticaria. Examples include raw seafood, latex, plant products. Latex allergies may cause anaphylaxis in certain individuals.
- Idiopathic: an underlying cause cannot be indentified
NOTE: Scombroid syndrome refers to development of flushing, urticaria, diarrhoea, headache, and sometimes bronchospasm following ingestion of poorly preserved fish (e.g. tuna, mackerel, sardines) that contain large amounts of histamine. May resemble an IgE-mediated reaction.
Chronic urticaria
Chronic urticaria may be inducible by physical stimuli such as heat, cold, vibration, dermographism, delayed pressure, aquagenic. In chronic spontaneous urticaria may be associated with an underlying disorder such as an atopic condition (e.g. atopic dermatitis, allergic rhinitis) or autoimmune disorder (e.g. thyroid disorders, coeliac disease, Sjögren syndrome, systemic lupus erythematosus). The association with malignancy is less clear.
Chronic spontaneous urticaria can also be aggravated or exacerbated by a number of factors:
- NSAIDs
- Environmental: heat, cold, sunlight
- Alcohol
- Opiate medications
- Stress
- Infections
- Physical pressure
Clinical features
Characteristically, urticaria presents with a red, raised, itchy rash.
The presentation of urticaria may be highly variable. Lesions are classically erythematous and itchy. They are often raised ranging from a few millimetres to several centimetres in size. This will give the appearance of multiple papules or plaques. Lesions often evolve rapidly, but will disappear within 24 hours. It may be difficult to appreciate the redness of lesions on darker skin.
Features
- Pruritic
- Erythematous appearance
- Rounded or irregular shape
- Multiple papules (< 1 cm) or plaques (> 1 cm)
- Lesions may coalesce
- Single area of the body or widespread
- With or without angioedema (usually localised)
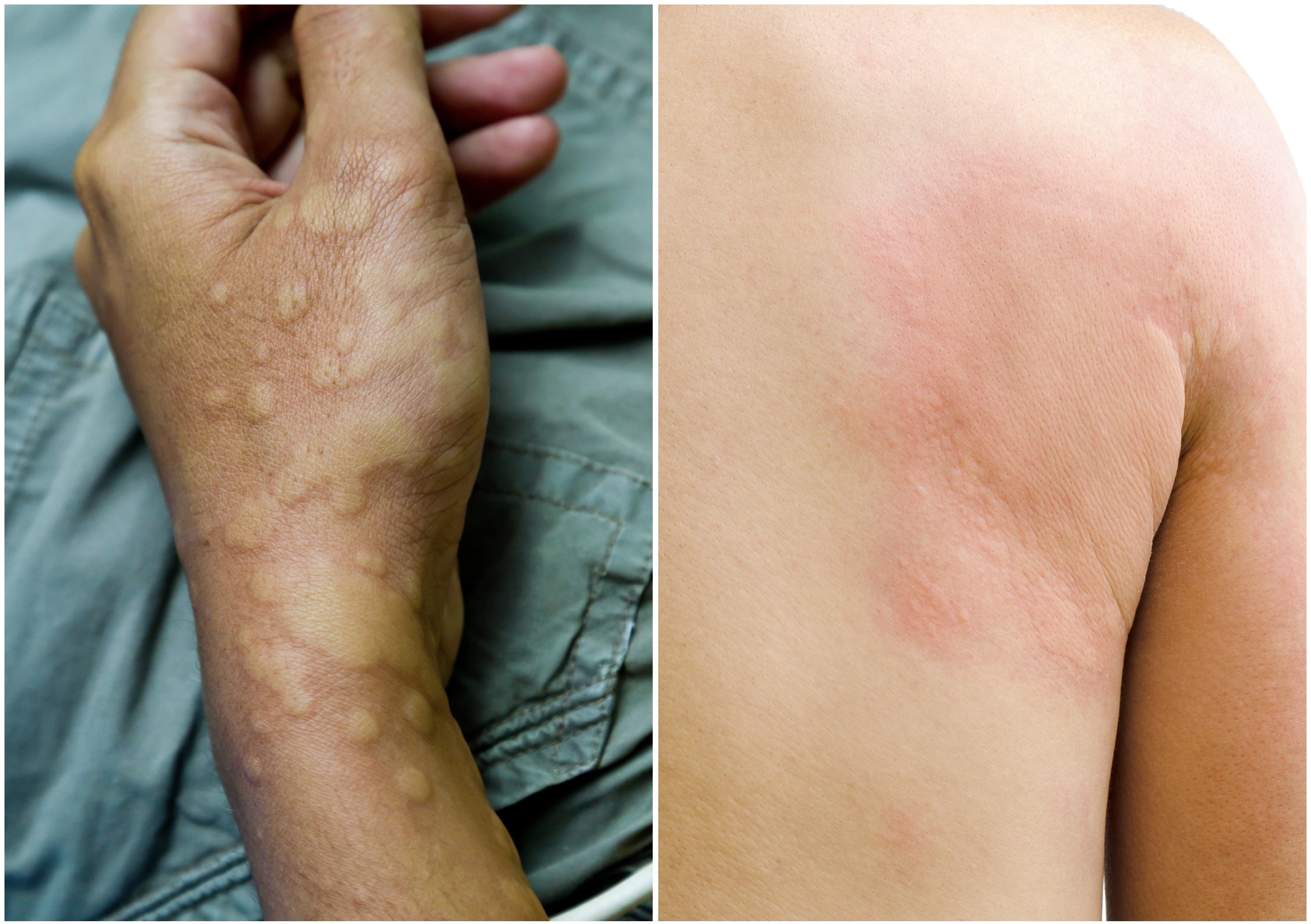
Typical examples of urticaria
Diagnosis & investigations
The diagnosis of urticaria is made clinically based on the presence of the characteristic skin lesions.
A definitive diagnosis of urticaria can be made with direct visualisation of the lesions. It is important to enquire about signs and symptoms of a generalised allergic reaction (e.g. chest tightness, shortness of breath, throat tightness, nausea, vomiting, abdominal pain, lightheadedness, etc).
If there are features of a systemic allergic reaction then patients need urgent assessment and management. Anaphylaxis is a life-threatening condition.
The underlying aetiology may be apparent from the history (e.g. insect bite, new medication). It is important to explore events leading up to the presentations during the history. This may include:
- Recent illnesses
- New medications
- Food ingestion
- Exercise/physical exertion
- Insect bites/stings
- Travel history
In general, if there is no suggestion of an underlying disorder, then formal laboratory investigations are not required. If there is suggestion of an allergic-reaction then patients can be referred to allergic or immunology clinic for further testing (e.g. allergen-specific IgE antibodies and/or skin prick testing).
Management
The majority of new-onset urticaria is self-limiting but the principle treatment is with anti-histamines.
It is critical that all patients presenting with urticaria are assessed for a more systemic allergic reaction (e.g. anaphylaxis) or angio-oedema affecting the airway due to laryngeal oedema. In these cases, patients need urgent management and referral to hospital for life-saving treatment and/or airway management.
In the absence of anaphylaxis or airway involvement, patients are predominantly managed with second generation anti-histamines (e.g. cetirizine, loratadine, fexofenadine).
Conservative
A large proportion of cases of urticaria will resolve spontaneously without need for intervention. Advice on avoiding any specific trigger or stopping culprit medications is important. If an allergic reaction (e.g. IgE-mediated) is suspected then patients should be referred to an allergic clinic for further assessment. This is because of the future risk of a more generalised allergic reaction.
Anti-histamines
Anti-histamines form the principal management of urticaria. There are two main groups of H1-receptor anti-histamines:
- First-generation: diphenhydramine, chlorpheniramine, hydroxyzine
- Second-generation: cetirizine, loratadine, fexofenadine
Second-generation agents are less-sedating, have almost no anti-cholinergic side-effects and less drug interactions. These medications also require less frequent dosing, which is preferable for patients. Patients may require higher than ‘standard doses’ to control symptoms. Anti-histamines are usually continued until lesions resolve.
Corticosteroids
Corticosteroids such as prednisolone or hydrocortisone are not required for isolated urticaria. They may be considered in patients with predominant angio-oedema symptoms (often given as a single dose of prednisolone unless laryngeal involvement). Occasionally, a short course (5-7 days) of steroids may be used in patients who are refractory to anti-histamines but long-term use is inappropriate and repeated courses should not be used.
Chronic spontaneous urticaria
Patients with chronic spontaneous urticaria usually require long-term use of second generation H1-receptor anti-histamines. High doses and use of additional agents (e.g. First-generation H1-receptor anti-histamines, leukotriene-receptor antagonists or H2-receptor anti-histamines) may be required.
Patients with refractory symptoms to oral medications may require systemic immunosuppression. Examples include Omalizumab (monoclonal antibody to IgE), cyclosporin or tacrolimus.
Last updated: March 2022
Have comments about these notes? Leave us feedback
