Tremor
Notes
Overview
A tremor is considered involuntary, rhythmic, oscillatory movements of a body part.
A tremor is considered the involuntary shaking of a body part. This is classically associated with the hand but can affect other parts of the body. This shaking may be defined as rhythmic, oscillatory movements (i.e. move back and forth) that occur due to alternating or synchronous contractions of opposing muscle groups.
Two key terms when describing tremor are frequency and amplitude:
- Frequency: this is essentially how quick the tremor is, or in other words, the oscillations (back and forth movement) per second. It is measured in cycles per second (Hertz - Hz). A low-frequency tremor is often 3-4 Hz (e.g. cerebellar tremor), whereas a high frequency is 10-12 Hz (e.g. physiological tremor)
- Amplitude: this is essentially the amount of movement, or in other words, the degree of displacement of the limb or body part. Large amplitude tremors (i.e. associated with more movement) are usually more disabling
Movement disorders
Tremor is considered the most common movement disorder.
Movement disorders are divided into two conventional types:
- Hyperkinetic: excess involuntary movement. Also known as dyskinesias
- Hypokinetic: evidence of slow or reduced movement. Parkinson’s disease is a classic hypokinetic movement disorder
These broad categories may be further divided into primary or secondary:
- Primary: the movement disorder is the main pathology
- Secondary: the movement disorder is secondary to another insult (e.g. metabolic, drugs)
Hyperkinetic
A variety of hyperkinetic movement disorders may be seen in clinical practice. Each of these hyperkinetic movements may be caused by a number of underlying conditions (e.g. infection, epilepsy, stroke):
- Chorea: brief, irregular contractions. Movement is not repetitive or rhythmic
- Dystonia: sustained or intermittent contractions. Often cause abnormal, repetitive movement and/or posturing
- Myoclonus: brief, shock-like contractions
- Stereotypies: repetitive, simple movements that can be voluntarily suppressed (e.g. chewing, rocking)
- Tics: repeated, intermittent movements. Usually briefly suppressible and associated with an urge to perform
- Tremor: rhythmic, oscillatory movements
Hypokinetic
Hypokinetic movement disorders essentially refer to a reduced or absent voluntary movement that is unrelated to weakness or spasticity. Spasticity is abnormal muscle tightness due to prolonged contraction. It is commonly seen after stroke or in cerebral palsy. Parkinson’s disease is the most well-known hypokinetic movement disorder.
Major features of hypokinetic movement disorders include:
- Akinesia: Inability to initiate voluntary movement
- Bradykinesia: Slowness of initiation of voluntary movement
- Rigidity: Resistance to passive movements. Resistance is velocity independent
Differential diagnosis
Tremors may be broadly divided into rest and action.
There are various ways to characterise tremors including the tremor frequency, area of the body affected or underlying cause. However, the most frequently used is the activating condition. In other words, whether it is precipitated by rest or action.
A tremor may be isolated (e.g. essential tremor) or combined alongside other neurological features (e.g. Parkinson’s disease).
Rest tremors
These tremors occur in a body part that is relaxed, fully supported against gravity and not voluntarily activated. The most classic cause of rest tremor is Parkinson’s disease. The degree of the tremor movement may fluctuate and its appearance may vary depending on how relaxed the patient is amongst other factors.
Rest tremors do not occur during voluntary activity, however, they may quickly reappear when the affected body part is placed into a new resting position. In addition, the tremor may be enhanced by asking the patient to perform a repetitive task with the opposite limb (e.g. wave left arm up and down) or perform a cognitive task (e.g. says the months backwards).
Causes of rest tremors include:
- Parkinson’s disease: classically presents with a unilateral ‘pill-rolling’ tremor that affects the hand with a frequency of 4-6 Hz. Less commonly may affect one foot/leg. Over time, may progress to involve other limbs and as the disease progresses the tremor tends to become more continuous, proximal and increase in amplitude
- Parkinsonism: any cause of Parkinson-like symptoms (e.g. anti-dopaminergic medications, Parkinson-plus syndromes, cerebrovascular disease). The typical presentation is with bilateral symptoms compared to the unilateral presentation in idiopathic Parkinson’s disease
- Rubral tremor: usually due to a midbrain lesion. It May be seen as a mixture of tremors (e.g. rest and action)
Action tremors
These tremors occur when there is voluntary muscle contraction. They can be further divided into different three subtypes:
- Kinetic tremors: occur during any voluntary movement. It May be consistent throughout the movement (simple) or increase as the affected body part reaches its target (intention)
- Postural tremors: occur when a specific posture is voluntarily maintained (e.g. holding an outstretched hand)
- Isometric tremors: occur when there is contraction against a stationary object (e.g. holding a cup)
To elicit an action tremor patients are often asked to perform a series of tasks. There are many different types of action tremors that may be precipitated by different actions.
Causes of action tremors include:
- Physiological tremor: a low amplitude, high-frequency tremor at 10-12 Hz may be observed in normal individuals. However, under ordinary circumstances, it is usually not visible. Many factors may enhance the tremor leading to its being observed, which is usually related to increased sympathetic activity (e.g. medications - beta-agonists, anxiety, fear, alcohol withdrawal, toxins - lithium toxicity)
- Essential tremor: this is a common neurological disorder affecting 1% of the population. Causes a low amplitude, high-frequency postural tremor that is usually bilateral. Most commonly affects the hands/arms in certain postures (e.g. held outstretched). A worse tremor with larger movements can be seen and other body parts may be affected including the head, voice, and trunk. Classically gets better with small amounts of alcohol
- Cerebellar tremor: this describes a tremor that occurs due to cerebellar pathology (e.g. chronic alcoholism, tumour, stroke, multiple sclerosis). Cerebellar tremors may vary but are classically described as an ‘intention tremor’ that increases as the body part (e.g. finger) reaches its target. This is observed during finger-nose testing. May be seen alongside dysmetria (inability to execute complex movements, usually because the judgement of distance is impaired) and ataxia (poor fine motor coordination) that help localise the tremor to the cerebellum. Typically low frequency 3-4 Hz and large amplitude
- Primary writing tremor: this refers to a tremor that is particularly severe during the action of writing but not other activities. Usually seen as a large amplitude of supination and pronation with a frequency of 5-6 Hz. Commonly seen alongside ‘writer’s cramp’, which is a dystonia (abnormal muscle contraction) of the hand muscles during writing
- Rubral tremor: usually due to a midbrain lesion. It May be seen as a mixture of tremors (e.g. rest and action)
NOTE: patients may have a functional, or psychogenic tremor, which is usually a complex mixture of tremors that produces disability out of proportion of the tremor, is changeable, and commonly treatment-resistant. There is typically variability in tremor frequency on examination.
History
The age of onset and evolution of tremor is important to aid the diagnosis.
The appearance of tremor may be very classical (e.g. occurs only during times of stress or anxiety) making the diagnosis straightforward. In other cases, it can be more difficult to differentiate between the different types and underlying causes. This is why a detailed history is very important in the assessment of tremors.
Firstly, does the tremor occur at rest or during an action? This should help to make the simple differentiation between rest tremors and action tremors. If during an action, is it related to a particular posture, action, or a mixture. For example, if it only occurs during writing this may suggest primary writers tremor, if it only occurs on outstretched arms it may suggest an essential tremor. The most commonly observed tremors are action, of which physiological and essential tremors are the most frequent.
In physiological tremors, there is usually a precipitating factor such as stress, medication, or underlying disease (e.g. hyperthyroidism). It is important to ask about other neurological features (e.g. slurred speech, focal neurological deficits, shuffling gait) that may point towards a cerebellar pathology or Parkinson’s disease. Ask about any new medications that have been started, especially ones known to precipitate a physiological tremor or Parkinson’s disease.
Family history is important, especially for essential tremor that often shows an autosomal dominant pattern of inheritance.
Examination
The examination is important to look for other neurological signs that could suggest a more global neurological problem.
Tremor is usually an obvious clinical sign so it is important to observe the tremor during the examination. Think about the frequency and amplitude of the tremor. There are complex ways of measuring these, but simple estimates can be useful (e.g. is the back and forth movement quick or slow, are the movements large or small).
While the hand and arms are commonly affected in many tremors, make sure you assess other body parts as well (e.g. legs, head). Essential tremor may affect the head leading to a vertical ‘yes-yes’ or horizontal ‘no-no’ type of tremor. Additionally, ask the patient to hold a note for a period of time, this may reveal a voice tremor that is also seen in essential tremor.
Observe what happens to tremors in different postures. If they occur at rest ensure you ask the patient to perform a distracting movement (e.g. move opposite limb up and down) or concentration task (count backward from 20) to exacerbate the tremor and make it easier to observe. Look at the tremor with the hand outstretched (e.g. postural) and what happens during a specific action (e.g. finger nose movements).
Finally, perform a full neurological examination and look for other signs of neurological disease (e.g. bradykinesia, slow shuffling gait, and postural instability in Parkinson’s disease).
Investigations
Basic investigations are important, especially when physiological tremors are suspected.
Basic investigations into a tremor may include blood tests and imaging:
- Bloods: full blood count, renal function, thyroid function tests, caeruloplasmin for Wilson’s disease, heavy metals or drug levels (if suspected)
- Imaging: magnetic resonance imaging (MRI) of the brain
Imaging may not be required if the presentation is classic for essential tremor, Parkinson’s disease, or physiological tremors. However, if there is uncertainty or an underlying neurological disorder is suspected then an MRI of the brain can be considered.
Key tip
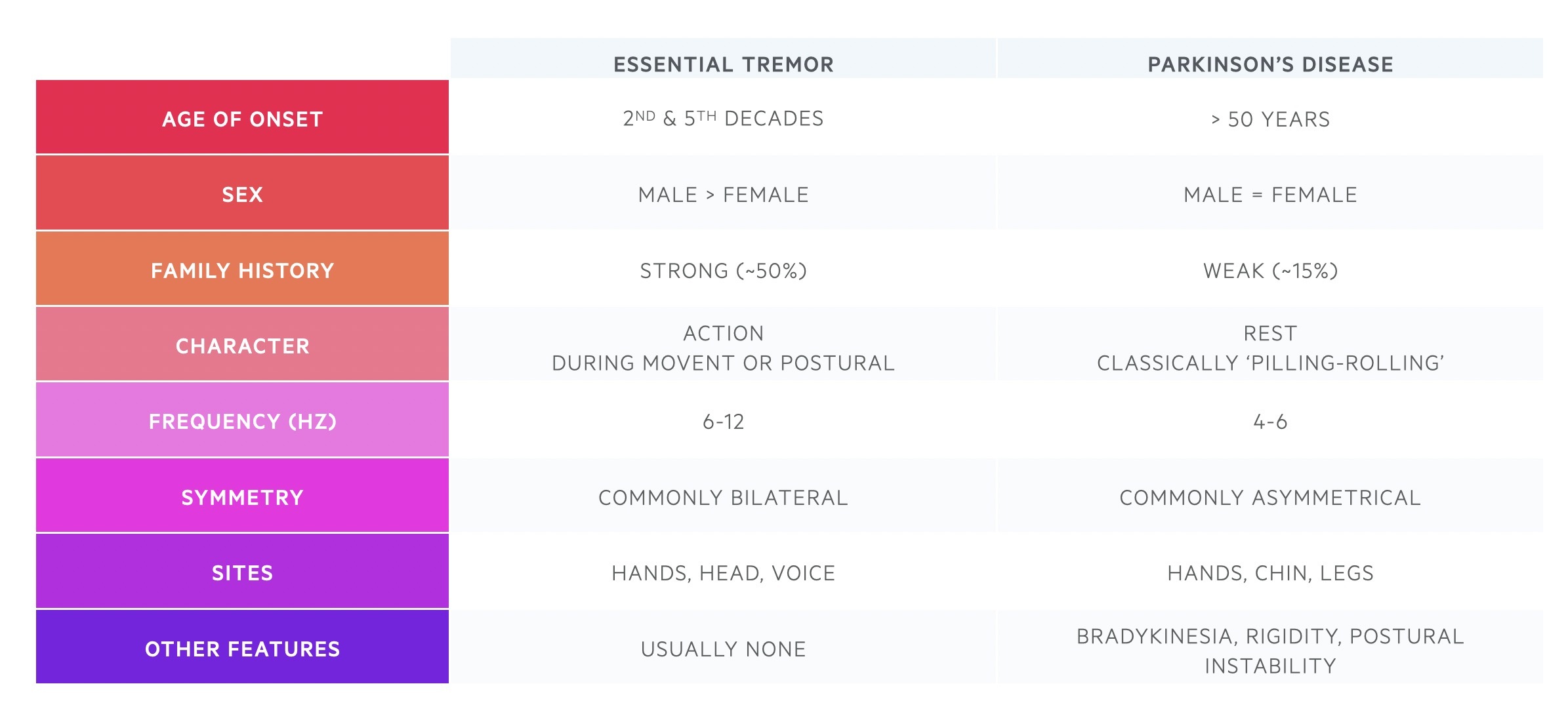
It is important to be able to differentiate between essential tremor and Parkinson’s disease.
The key differences between essential tremor and Parkinson’s disease are shown in the table below.
Last updated: June 2022
Have comments about these notes? Leave us feedback
