Syphilis
Notes
Overview
Syphilis refers to an infection caused by the bacterium Treponema pallidum.
Syphilis is predominantly a sexually transmitted infection (STI) caused by the bacterium Treponema pallidum. Transmission occurs from direct contact with infectious lesions, usually during sexual intercourse.
Untreated, syphilis can affect almost any organ in the body and was traditionally called the ‘great imposter’ because it can mimic many diseases in its late stages. Before the era of antibiotics syphilis was very common but it is now easily treated with penicillin when detected.
Epidemiology
The prevalence of syphilis has been growing in the UK over the last decade.
Traditionally, Syphilis was a common condition but the incidence dropped with the widespread introduction of antibiotics in the 1940s. Since then, incidence has varied, but sustained growth since 2000 has been seen with a significant increase in cases in the UK between 2013-2018. Worldwide there were >19 million cases of syphilis in 2016.
New cases are most common in young adults (aged 20-29 years) and >75% of cases in 2018 were among men who have sex with men (MSM). Among MSM, up to 40% with syphilis have co-infection with human immunodeficiency virus (HIV). In addition, almost 50% of MSM with syphilis were diagnosed with another STI during the same episode or within the previous year.
Microbiology
Treponema pallidum is a spirochete microorganism that is solely a human pathogen.
T. pallidum was first discovered in the 20th century. It is a spirochete microorganism that has a tight spiral-shaped structure and can be seen on dark field microscopy. It is too slender to be seen on routine microscopy and although it can be considered a gram-negative organism it is not seen on gram-stain.
Stages of disease
Syphilis can be categorised into four stages known as primary, secondary, latent and tertiary.
Syphilis is categorised into four stages:
- Primary
- Secondary
- Latent: divided into early latent and late latent
- Tertiary
Syphilis may also be categorised into early and late:
- Early: primary, secondary or early latent syphilis
- Late: late latent and tertiary syphilis
Primary
Characterised by development of a painless ulcer known as a chancre. Develops at the site of inoculation. May go unnoticed depending on the site of infection (e.g. posterior pharynx) and may be associated with lymphadenopathy.
Incubation period (time from infection to development of chancre) is 3-90 days (mean 21 days). Usually resolves in 3-10 weeks.
Secondary
Highly variable stage seen in approximately 25% of untreated patients (i.e. 1 out 4 patients who are not treated for primary syphilis). It is characterised by a systemic illness with multiple clinical features. Usually develops 4-12 weeks after appearance of the chancre and resolves within 3-12 weeks.
Latent
An asymptomatic period in which there is serological evidence of infection but no symptoms. Divided into early or late latent syphilis:
- Early latent syphilis: < 2 years from infection
- Late latent syphilis: > 2 years from infection
Tertiary
Since the era of antibiotics, tertiary syphilis is rare. Most commonly develops 15-40 years following infection. It is characterised by cardiovascular syphilis (e.g. aortitis, aortic regurgitation, heart failure), Gummatous syphilis (granulomatous lesions most commonly seen in the skin and bone) and neurosyphilis.
Late neurosyphilis is characterised by two presentations:
- General paresis: affects the cerebral cortex. Presents with dementia-type picture, personality change, seizures and motor defects.
- Tabes dorsalis: affects the dorsal columns of the spinal cord. Presents with paraesthesia and dorsal column changes (abnormal proprioception, abnormal vibration, abnormal sensation, upgoing plantars, absent ankle jerks).
Congenital syphilis
Syphilis infection increases the risk of miscarriage and stillbirth.
Congenital syphilis refers to a child born with the condition due to vertical transmission between mother and fetus. Divided into two types:
- Early: presenting < 2 years after birth. Typically presents with rash, haemorrhagic rhinitis ('bloody snuffles'), lymphadenopathy, skeletal changes and hepatosplenomegaly. Many other features can be present.
- Late: presenting > 2 years after birth. Persistent inflammation predominantly affects bones and teeth leading to characteristic features (see clinical features).
Aetiology & pathophysiology
Syphilis is caused by T. pallidum, which is able to penetrate mucus membranes or pass through skin abrasions.
Syphilis is due to infection by the spirochete T. pallidum, which is most commonly sexually transmitted. As such, syphilis is normally checked as part of a STI work-up.
Transmission
The organism can be transmitted by direct contact with infectious lesions, between mother and fetus or sharing needles among those who inject drugs.
- Direct contact with infectious lesions: contact with the chancre of primary syphilis (a painless ulcer) or infectious lesions of secondary syphilis can transmit the organism.
- Vertical transmission: the organism can be transmitted between mother and fetus during pregnancy because the bacteria easily cross the placenta. Screening for syphilis is part of antenatal care in the UK.
- Sharing needles: intravenous drug users can acquire syphilis from contaminated needles.
Early syphilis
T. Pallidum is able to penetrate mucous membranes or pass through skin abrasions. At the site of inoculation a small papule develops, which progresses to a painless ulcer known as a chancre that is highly infectious. The chancre is most commonly located in the genital region, but can occur at any area depending on the site of contact and it may be hidden to the patient (e.g. pharynx, anus, or vagina).
The incubation period ranges from 3-90 days (Median 21 days). There is a local infection, which can spread to regional lymph nodes and may disseminate. Around 25% of untreated patients will develop a more systemic illness weeks to months (e.g. 4-12 weeks) following infection known as secondary syphilis. Secondary syphilis is characterised by a variety of clinical features (see below) and is highly variable.
Late syphilis
Late syphilis is also highly variable and may develop 1-30 years following initial infection. There may be a long latent period before clinical features develop. Around 25-40% of untreated patients can develop late disease. Patients with late syphilis do not necessarily need to have had clinically symptomatic primary or secondary syphilis.
Clinically, late syphilis is characterised by:
- Cardiovascular syphilis (80-85%)
- Gummatous syphilis (late benign)
- Neurosyphilis (5-10%)
Within the cardiovascular system, syphilis is characterised by endarteritis (inflammation of arteries) and there is a delayed-type hypersensitivity reaction with an incomplete immune response. Aortitis (inflammation of the aorta) is classic of cardiovascular syphilis, which can lead to complications such as aortic regurgitation and heart failure.
In the central nervous system, there is infiltration of the cerebrospinal fluid (CSF) with T. pallidum. Spontaneous clearance can occur. However, without clearance there is risk of ongoing inflammation and subsequent ‘symptomatic neurosyphilis’. Symptomatic neurosyphilis may occur in secondary syphilis (e.g. meningitis, cranial nerve palsies) or tertiary syphilis (e.g. General paresis and tabes dorsalis).
Clinical features
Primary syphilis is characterised by development of a single, painless, indurated ulcer known as a chancre.
Primary
- Chancre: starts as a painless small papule, which subsequently ulcerates forming a solitary, indurated, painless ulcer. Typically 1-2 cms in size. Multiple may occur in the presence of HIV.
- Lymphadenopathy: regional to the site of the chancre.
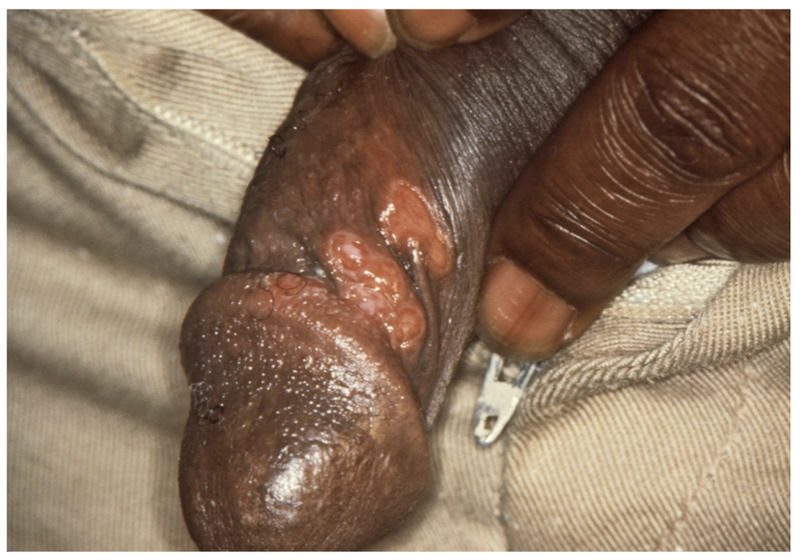
Chancre of primary syphilis located on the penile shaft
Image courtesy of the CDC
Secondary
Presentation is variable between patients and usually multi-system. There may be no preceding history of a chancre.
- Generalised: fever, headache, myalgia, malaise, anorexia, sore throat and/or weight loss.
- Dermatological (90%)
- Systemic rash: diffuse, symmetrical macular or papular eruption that spreads to involve trunk and extremities including the palms and soles. Individual lesions are usually 0.5-2cm in size and reddish-brown.
- Alopecia (hair loss): can develop a ‘moth-eaten’ alopecia affecting scalp, beard or eye-brows.
- Condylomata lata: infectious grey/white warty lesions. Usually found in orogenital regions.
- Mucous patches (‘snail-tract lesions’): ulcerative patches can occur in the orogenital regions. Appear as oval-shaped swallow ulcers.
- Gastrointestinal: Hepatitis, splenomegaly and ulcerated GI lesions.
- Musculoskeletal: Synovitis, osteitis (inflammation of bone) and periostitis (inflammation of periosteum of bone).
- Ophthalmic: uveitis, optic neuropathy and retinitis may occur. More common with HIV co-infection.
- Neurological (1-2%): meningitis (e.g. headache, neck stiffness, photophobia), cranial nerve palsies (8th & 2nd) and hearing loss.
Tertiary
- Cardiovascular syphilis (10-30 years following infection): chest pain, shortness of breath and palpitations may develop due to aortitis, aortic regurgitation and heart failure. Clinically may have an early diastolic murmur.
- Gummatous syphilis (very uncommon, ~15 years after infection): refers to presence of gumma, which are granulomatous nodules with central necrosis and can occur anywhere. Most common in skin and bones.
- Neurosyphilis
- General paresis (10-20 years after infection): also known as 'general paralysis of the insane', 'paretic neurosyphilis', or 'dementia paralytica'. Dementia-type illness with gradual decline in memory, cognitive function and personality change. Seizures and hemiparesis can occur.
- Tabes dorsalis (15-25 years after infection): most common form of neurosyphilis before era of antibiotics. Characterised by paraesthesia, lightning pains, loss of light touch, proprioception and vibration sense due to dorsal column involvement. Causes absent ankle reflex with upgoing plantars. May also develop optic atrophy and pupillary abnormalities*.
*NOTE: Argyll-Robinson pupil is seen in Tabes dorsalis and refers to a mitotic (small) pupil that accommodates but does not react to light. May be unilateral or bilateral.
Congenital
Early congenital syphilis may have clinical features similar to severe secondary syphilis in adults.
Late manifestations predominantly affect bone and teeth with some classic clinical signs:
- Saddle nose: nasal septum destruction
- Saber shins: bowing of tibia from chronic inflammation
- Clutton’s joints: symmetrical joint swelling. Most commonly the knees
- Hutchinson’s teeth: widely spaced and notched upper incisors
- Mulberry molars: molar teeth with too many cusps
Diagnosis
Syphilis is diagnosed using serological tests.
Serological testing is used to make a diagnosis of syphilis. It is based on the interpretation of two tests:
- Nontreponemal tests
- Treponemal-specific tests
Various laboratory algorithms are available that dictate which tests should be completed first, and which are required as confirmatory tests.
Nontreponemal tests
This refers to two different tests:
- Rapid plasma reagin (RPR)
- Venereal Disease Research Laboratory (VDRL)
These are non-specific tests that assess serum reactivity to cardiolipin-cholesterol-lecithin antigen from an infected or suspected infected patient. Positive tests are reported as a titre (e.g. 1:32). Following treatment, the titre of antibody will fall allowing use in patients who have previously been treated for syphilis.
Treponemal-specific tests
This refers, but not limited to, the following tests:
- T. pallidum particle agglutination assay (TPPA)
- Fluorescent treponemal antibody absorption (FTA-ABS)
- T. pallidum enzyme immunoassay (TP-EIA)
Detects antibodies that react to specific treponemal antigens. They are more specific, but following infection with T. pallidum they remain reactive life-long, even if the bacteria have been cleared. Reported as a qualitative result (e.g. reactive or non-reactive). Often a screening treponemal test is completed first and then followed by a confirmatory test.
Who to test
Asymptomatic patients with high-risk sexual behaviour should be tested for syphilis.
Patients with signs and symptoms of syphilis should be tested for the disease. This includes patients presenting with primary, secondary or tertiary syphilis. For example:
- Primary: presentation with a chancre
- Secondary: presentation with the classic maculopapular skin rash
- Tertiary: presentation with heart failure or dementia
Alternatively, asymptomatic patients who are at high risk of acquiring the disease should also be tested. This includes:
- Contact with a person who has primary syphilis
- HIV-infected individuals
- Sexually active MSM
- High-risk sexual behaviour: other STIs, exchange sex for drugs/money, unprotected sex
- Routinely as part of a sexual health screen
Investigations
Any patient with a diagnosis of syphilis should also be tested for HIV.
Co-infection
Patients with suspected, or confirmed, syphilis should be tested for other STIs such as chlamydia, gonorrhoea and HIV. Patients should be referred to a genito-urinary medicine (GUM) clinic for treatment. A GUM clinic will help with contact tracing and advice on safe sex.
Additional investigations
The role of additional investigations (e.g. bloods, imaging, special tests), depend on the clinical presentation and co-morbidities. Patients with secondary syphilis may need more comprehensive blood tests sending due to the systemic involvement of the illness. In addition, investigations should be tailored to the presenting problem (e.g. hepatitis, meningitis).
Consider neuroimaging and lumbar puncture in patients with suspected neurosyphilis.
Management
The treatment of syphilis is with parenteral penicillin.
Patients with confirmed syphilis on serological testing or those with suspected syphilis based on clinical findings (e.g. chancre, recent exposure) can be given treatment.
Penicillin is the treatment of choice for syphilis, which is given to all stages. However, the dose and course length of penicillin is dependent on the stage.
Treatment recommendations
- Early syphilis:
- Benzathine penicillin 2.4 Million units, IM single dose.
- Late syphilis (cardiovascular or gummatous):
- Benzathine penicillin 2.4 million units, IM weekly for three weeks (3 doses)
- Prednisolone 40-60 mg for three days if cardiovascular (see Jarisch-Herxheimer reaction)
- Neurosyphilis:
- Procaine penicillin 1.8-2.4 million units IM once daily plus probenecid 500 mg QDS for 14 days, OR
- benzylpenicillin 10.8-14.4 g daily, given as 1.8-2.4 g IV every 4 hours for 14 days.
- Prednisolone 40-60 mg for three days (see Jarisch-Herxheimer reaction)
- Syphilis in pregnancy:
- Benzathine penicillin 2.4 million units IM single dose in the first and second trimesters. Further dose in the third trimester followed by a second dose after one week.
Penicillin allergy
In patients with a penicillin allergy always confirm the nature of the allergy. Some patients may have an intolerance rather than overt allergy and administration of parenteral penicillin may actually be appropriate.
It may be necessary to refer patients for allergy testing prior to initiation of treatment. In those with a confirmed allergy, alternative antibiotics choices can be used including doxycyline, ceftriaxone, azithromycin or erythromycin. This is guided by GUM specialists.
Jarisch-Herxheimer reaction
This refers to an acute febrile illness that usually presents within the first 24 hours of treatment for syphilis with headache, myalgia, chills and rigors.
The reaction occurs after the initial dose of anti-treponemal treatment. It occurs in 10-35 % of patients and is most common in early syphilis. It usually self-resolves without intervention in 12-24 hours. Anti-inflammatory drugs can be used (e.g. NSAIDs).
Due to the potentially life-threatening nature of the reaction in patients with late tertiary cardiovascular or neurosyphilis, steroids are usually recommended (prednisolone 40-60 mg once daily). They are given for three days starting 24 hours before the initial dose of anti-treponemal antibiotics.
Last updated: June 2021
Further reading
British Association for Sexual Health and HIV (BASHH) guidelines.
Have comments about these notes? Leave us feedback
