Hand, foot and mouth disease
Notes
Definition & classification
Hand, foot and mouth disease (HFMD) is an acute viral illness, which is usually mild and self-limiting.
The disease is characterised by papulovesicular lesions on the distal limbs and vesicular eruptions in the mouth.
HFMD occurs worldwide. In temperate climates (including the UK) it is most common in late summer and early autumn. It presents either in outbreaks or as sporadic cases. Outbreaks occur frequently in schools and nurseries, and it often spreads within families.
It occurs most typically in children under 10 years of age, and most commonly in those under 4 years of age.
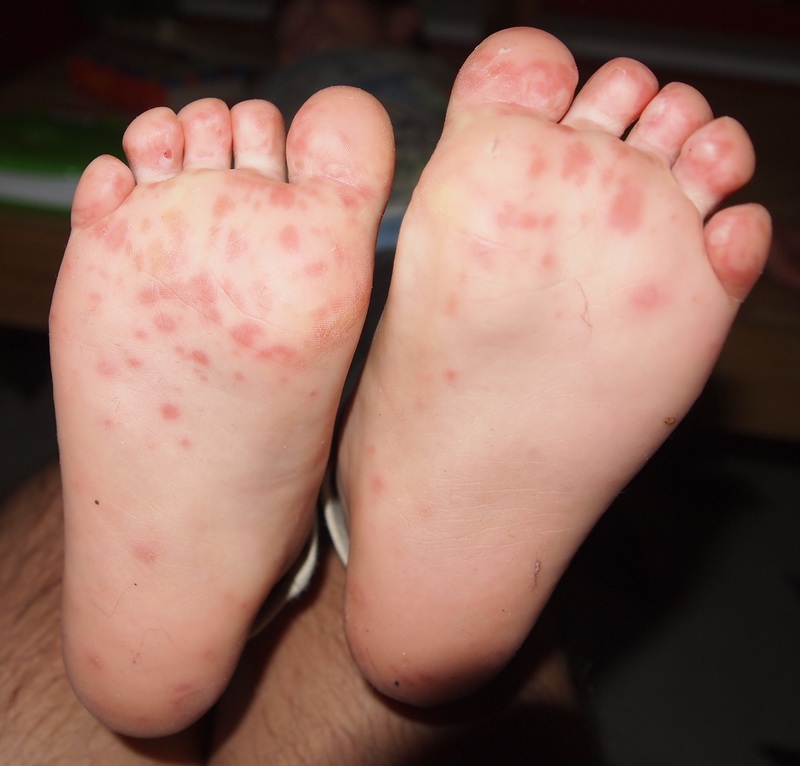
Hand, foot & mouth disease in a child. Image courtesy of Wikipedia Commons.
Aetiology & pathophysiology
HFMD is most commonly caused by Coxsackie A16 virus, but can also be caused by other group A and B Coxsackie viruses.
HFMD may also be caused by Enterovirus 71, which can lead to a more serious clinical picture. Importantly, HFMD is transmitted between humans and does not have an animal host. This means it is not transmited from or to animals, and has no relation to foot and mouth disease.
HFMD can be transmitted in the following ways:
- Direct contact with infected respiratory secretions (coughing and sneezing)
- Direct contact with fluid from the blisters
- Faeco-oral transmission. The virus can be faecally shedded for 4-8 weeks after the onset of the initial viral illness, therefore asymptomatic individuals can continue to infect others
- Vertical transmission from mother to foetus
Clinical features
HFMD is, in most cases, a mild and self-limiting disease.
Not all clinical features are present in every case, and not all children get lesions on their hand, feet or in their mouths. It has an incubation period of 3-7 days. There is a prodromal period (12-36 hours) of fever (38-39°C), malaise, decreased appetite, cough, abdominal pain and myalgia. If HFMD is caused by enterovirus 71, there may rarely be vomiting.
There are two types of lesion in HFMD - mouth lesions and distal limb lesions.
Mouth lesions
These generally appear first as 2-8 mm diameter erythematous macules and papules (commonly on hard palate, tongue and buccal mucosa). These progress rapidly to vesicles, which easily erode. The eroding vesicles leave shallow yellow-grey ulcers with an erythematous halo.
Distal limb lesions
The limb lesions appear soon after the oral lesions as 2-5 mm diameter erythematous macules and papules, often with a central grey coloured vesicle. The vesicles found on the limbs are often elliptical with the long axis running in parallel with the skin lines.
The limb lesions most commonly affect the sides of the fingers, dorsum of the hands and the margins of the heels. Less frequently they are seen on the heals and palms with the buttocks and groins occassionally being affected.
Atypical HFMD
Atypical HFMD has been described, and is caused by Coxsackie virus A6. It presents with nail shedding and more extensive and widespread skin disease.
Investigations & diagnosis
Diagnosis of HFMD is almost always clinical, based upon thorough history taking and recognition of clinical signs.
Laboratory identification of the virus causing the HFMD may be of value in outbreaks or special circumstances (such as late pregnancy when there is a risk of transmission to the foetus). It depends upon use of techniques such a polymerase chain reaction (PCR).
Management
Management is limited to offering supportive treatment and treatment of complications.
Reassurance to parents or carers is important. They may be confused about possible link with foot and mouth disease of animals, and the fact that the diseases are not related should be explained. Good hand hygiene and cleaning surfaces contaminated with bodily fluids should help prevent transmission.
Dehydration is the most common complication as the oral lesions are painful so oral intake is reduced. Ensuring regular analgesia and encouraging good oral fluid intake is the mainstay of treatment. If the lesions become secondarily infected, then antibiotic treatment may be necessary, but should not be routinely prescribed.
Enterovirus infection may rarely cause serious neurological complications, including aseptic meningitis, encephalitis, acute flaccid paralysis and neurogenic pulmonary oedema which can be fatal.
Once infected with one virus subgroup, immunity should exist, but it is always possible to get HFMD again if infected with a different virus of virus subgroup. There are no vaccines available for the viruses which cause HFMD.
Last updated: March 2021
Have comments about these notes? Leave us feedback
