Acute subdural haematoma
Notes
Definition
Subdural haematoma is a collection of blood in the subdural space.
Subdural haematoma (SDH) refers to a collection of blood in the subdural space. This is situated underneath the dura and above the arachnoid mater meningeal layers. There are several classifications of SDH:
- Acute (ASDH): bleeding occurring in the last 1-3 days.
- Chronic (CSDH). blood that has usually been present for > 3 weeks.
- Subacute: bleeding that occurs between 4 days and 2-3 weeks
- Acute on chronic: chronic haematoma that may expand secondary to recurrent bleeding
Aetiology
The most common cause of ASDH is trauma.
ASDH is often a life-threatening emergency and historically mortality figures have been as high as 68-90%. If appropriate, patients require emergency neurosurgery.
Mortality is often not due to the ASDH alone but several underlying factors such as the mechanism of injury, which is often a high impact injury (see list below). There may be other injuries such as a polytrauma or further significant intracranial injuries alongside the ASDH. Lastly, the patient may be taking an anticoagulant or antiplatelet medication, which can significantly affect the risk of bleeding.
Trauma
The most common cause of ASDH is trauma based on a cohort study spanning 20 years:
- Fall, less than 2m – 34%
- Fall, more than 2m – 24%
- Road traffic collision – 25%
In the trauma study, 74% of the patients were male with a median age of 48.9 years.
Non-trauma
- Intracerebral haemorrhage: bleeding may extend into the subdural space
- Rupture of cerebral aneurysm: can accompany up to 7.9% of aneurysmal subarachnoid haemorrhages
- Arteriovenous malformations
- Brain tumours
- Systemic thrombolysis
Risk factors
Patients with significant cerebral atrophy are at high risk for SDH. In these patients, trivial head trauma in the absence of physical impact may produce an ASDH. Patients likely to have cerebral atrophy include those with neurodegenerative diseases, chronic alcohol abuse or traumatic brain injury.
The risk factors associated with an ASDH include:
- Mechanism of injury (fall or road traffic collision)
- Anticoagulants/antiplatelet use
- Alcohol excess
- Liver dysfunction
- Coagulopathies
It is worth noting that the majority of patients with an ASDH causing significant mass effect (midline shift or herniation) will likely have a reduced Glasgow Coma Score (GCS) or be comatose and therefore likely to be non-communicative and compliant with examinations.
Anatomy & pathophysiology
The brain is encased in three meningeal layers: the dura, arachnoid and pia mater.
In order to understand the anatomy and consequences of a subdural haematoma (chronic or acute), we need to understand the anatomy of the meninges and the physiology of the Monro-Kellie doctrine.
Meninges
The brain is encased in three meningeal layers, which are the dura, arachnoid and pia mater (outside to inside). The pia mater is adherent to the surface of the brain and spinal cord. The subarachnoid space is found between the arachnoid and pia mater. The subdural space, a potential space, is found between the dura and arachnoid mater.
Pathophysiology
There is impact damage when an ASDH forms, which causes the bleed to be potentially lethal. There may be overlying skull fractures and underlying brain injury such as contusions or traumatic subarachnoid haemorrhage. An ASDH forms when there is a sudden tear of a surface or bridging vessel as a result of a rapid change from acceleration to deceleration forces.
Monro-Kellie doctrine
The Monro-Kellie doctrine states that the skull is a closed vault and the sum of the brain parenchyma, cerebrospinal fluid (CSF) and blood is constant. It is a pressure-volume relationship. If one increases, then either or both must decrease in order to compensate.
In the case of an ASDH, the presence of extra blood exerts mass effect and this can be potentially lethal as it can cause compression of the brainstem. Therefore, the operative management involves a procedure called a decompressive craniectomy or craniotomy to relieve pressure, evacuate the blood clot and stop the bleeding.
It is worth noting, the primary brain injury has already occurred by the time of presentation and management is aimed at minimising the impact of secondary brain injury.
Traumatic brain injury
ASDH falls under the umbrella term of traumatic brain injury.
An acute subdural haematoma complicates around 11% of mild to severe head injuries needing hospitalisation and around 20% of severe traumatic brain injuries (TBI).
Classification
TBI is a heterogenous term with many different ways to classify the injury (e.g. clinical severity, mechanism of injury). Traditionally, TBI is classified according to the Glasgow Coma Score (GCS).
- GCS (13-15): mild TBI
- GCS (9-12): moderate TBI
- GCS (≤ 8): severe TBI
Sequelae
Classic pathological injuries associated with TBI include:
- Skull fracture
- Subdural hematoma (SDH)
- Subarachnoid haemorrhage (SAH)
- Intraparenchymal haemorrhage
- Cerebral contusion
- Intraventricular haemorrhage
Clinical features
Patients with an ASDH usually present with a decreased level of consciousness.
Due to the reduced level of consciousness, patients with ASDH are usually non-communicative. If they had a significant trauma, they might already be intubated, ventilated and sedated pre-hospital.
Alert patients may have features of headache, vomiting or focal neurological deficits.
Symptoms
- Headache
- Nausea
- Vomiting
- Seizures
Signs
- Reduced level of consciousness (GCS)
- Focal neurological deficit (e.g. weakness)
- Anisocoria (unequal pupils)
- Signs of herniation (fixed and dilated pupil)
- CSF leak if concurrent skull fractures
Clinical examination
One can only perform a neurological examination if the patient is alert enough. If the patient has a reduced GCS or is already intubated, ventilated and sedated, the only clinical correlates for brain activity are pupillary response and intracranial pressure (ICP).
In the setting of brain trauma, ICP should be less < 22 mmHg. ICP monitors are usually inserted by neurosurgeons and not routinely inserted in a pre-hospital setting so this will usually not be available.
Glasgow Coma Scale
The Glasgow Coma Scale is a clinical scale used to reliably measure a person's level of consciousness after a brain injury.
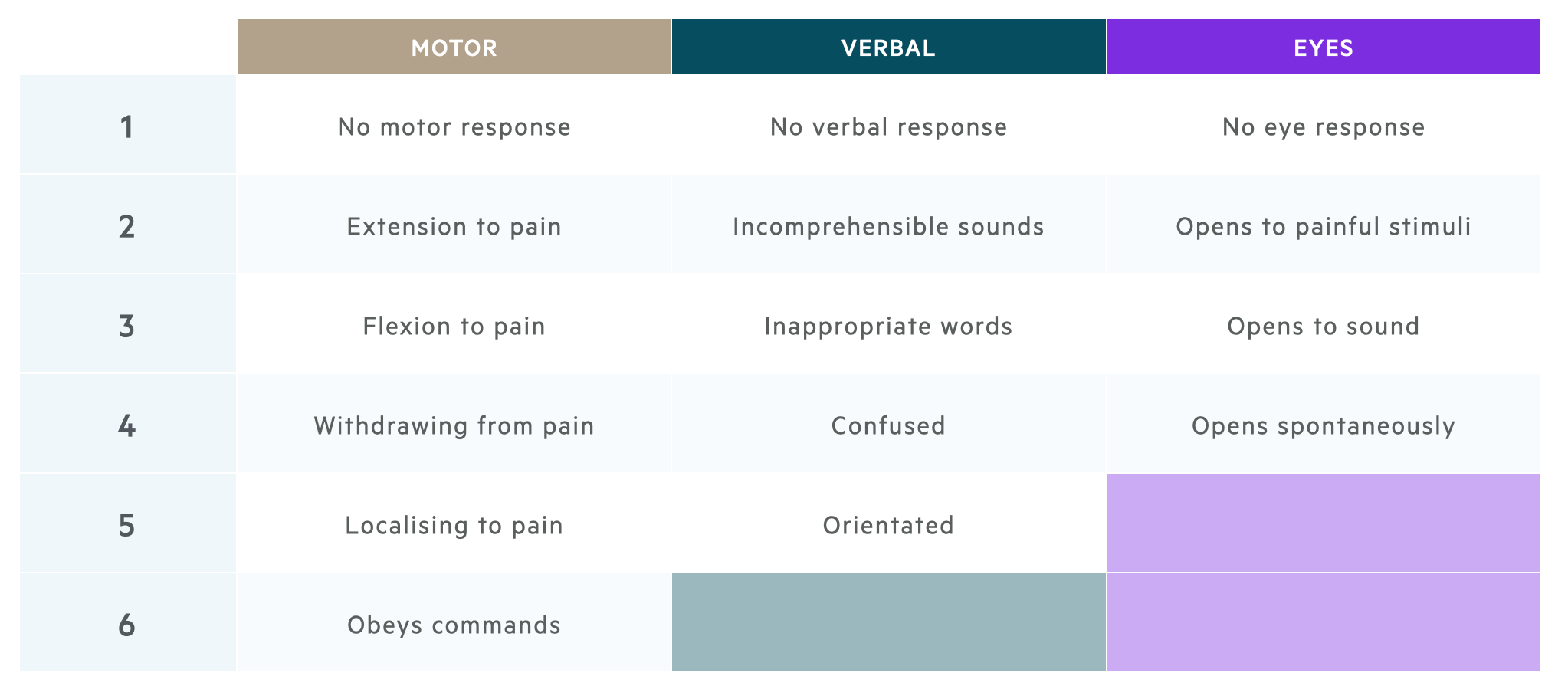
It is important to be familiar with the Glasgow Coma Scale (GCS) which is measured from 3 to 15 and has three elements.
- Motor response (1-6)
- Verbal response (1-5)
- Eye response (1-4)
Please remember, the best possible score in each category is recorded and one has to adapt (for instance, if the patient has weakness on one side, you can assess obeying commands by asking the patient to stick out their tongue).
Diagnosis
An urgent CT head is the investigation of choice for the diagnosis of ASDH.
The diagnosis of an ASDH is rooted in the history (e.g. trauma) and examination (e.g. reduced GCS). This being said, the principle investigation is a non-contrast CT head that will clearly show blood within the subdural space.
Acute SDH is readily seen on a non-contrast CT head as a high-density crescentic collection. This will usually be part of the trauma series if the patient is a ‘trauma call’. Otherwise a CT Head and CT Neck should be ordered. It is always good practice to obtain CT Neck imaging in trauma cases as there are often concurrent injuries which may require a collar and also aid neurosurgeons with operative planning. Subacute and chronic SDH will appear as isodense or hypodense crescent-shaped lesions on CT.
A large or rapidly expanding SDH may show mass effect with distortion of the normal anatomy. This may be less obvious with bilateral haematomas.
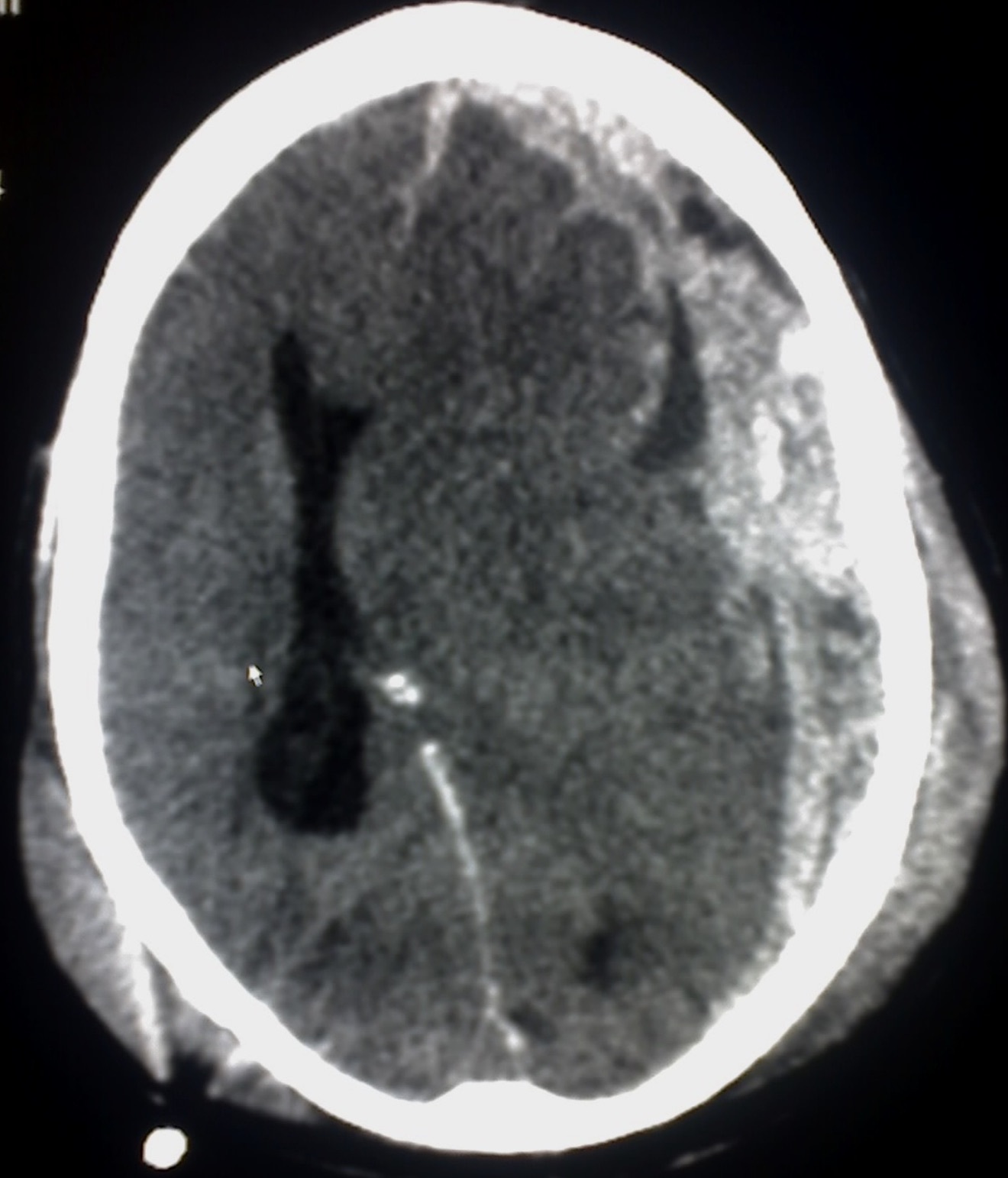
CT head showing an acute left-sided subdural haematoma
(notice the high density white material)
Investigations
Investigations are critical to work-up patients with a suspected ASDH to enable planning for surgery (if required), assessing for sequelae of trauma (if present) and determining the aetiology (if unknown).
Bedside
- Neurological observations: monitoring of GCS
- Blood glucose
- ECG
Bloods
- FBC - check for anaemia and thrombocytopenia
- U&E - check the electrolytes, especially sodium
- LFT - disorder or history of alcohol abuse
- Bone Profile - check for calcium
- Coagulation - check for clotting disorder
- G&S - consider if going for surgery
- Crossmatch - for blood products such as FFP, platelets and packed red blood cells
Imaging
Many patients presenting with trauma may undergo a full trauma series, which can include a CT head, neck, chest, abdomen and pelvis.
Indications for performing a trauma series will vary depending on the trauma centre, but typical indications include:
- High speed motor vehicle collision
- Non-trivial motorcycle collision
- Fall from height >2 metres
- Other concerning mechanism of injury
Management
The management of ASDH has several key elements: resuscitation, initial management, medical management and surgical management.
Resuscitation
In the first instance, patients with an ASDH require resuscitation. This is usually completed as part of the initial 'trauma call'.
A trauma call is an alert to the 'trauma team' to quickly assemble in response to a major trauma. The team usually consists of a team leader (accident & emergency trauma consultant) alongside an anaesthetic registrar, general surgery registrar, orthopaedic registrar, neurosurgical registrar and accident & emergency nursing team. The team will complete a rapid assessment following the mnemonic (C)ABCDE with attention paid to control of any catastrophic bleeding urgently. The patient is stabilised, undergoes urgent investigations (e.g. blood gas) and will usually have a CT trauma series. An ASDH may be suspected clinically and will be detected on CT.
Stabilisation involves control of any further sources of bleeding, any coagulopathies and any acid-base disturbances. If other systems are compromised such as breathing, chest drains may be inserted or pelvic binders may be applied. It is important to remember a patient usually won’t be rushed for surgery until they are stable to be transferred to the scanner and theatre.
Initial management
Patients with an ASDH can present alert or in a coma. This is assessed using the Glasgow Coma Score. A systematic ABCDE is utilised in emergency settings. If the patient has a low GCS (< 8) they will require airway management.
Medical management
A patient presenting with a suspected ASDH should be monitored closely with neuro-observations. The primary concern is secondary brain injury and therefore neuroprotective parameters are used to manage intracranial pressure (ICP).
Not every ASDH is amenable to surgical management and therefore polytrauma patients may be managed conservatively. Where patients are managed depends on the severity of injuries and need for intubation and ventilation. On intensive care patients can have closer monitoring of ICP.
Neuroprotective measures:
- Normoxia (maintaining normal oxygen saturations)
- Normocarbia (carbon dioxide can be altered it ventilated)
- Normothermia (maintain normal temperature)
- Adequate sedation and paralysis
- Intracranial pressure (ICP) monitoring: ensure < 22 mmHg
As part of management, collars may be loosed or the patient sat up to 30 degrees but this requires discussion with neurosurgery with due consideration to any further injuries.
ICP management:
Medically, ICP can be managed using hypertonic saline 2.7% or mannitol. Mannitol is not commonly used but may still be mentioned in guidelines. These agents do not cross the blood brain barrier and are able to draw out CSF and reduce ICP.
Seizure management:
Agents such as levetiracetam (Keppra) may be given to manage any seizure activity due to direct cortical irritation by blood.
Surgical management
Urgent neurosurgical intervention may be warranted in the following situations:
- Significant mass affect or midline shift
- Fall in GCS
- Anisocoria
- Fixed & dilated pupils
- Persistently raised ICP
Patients require decompressive surgery to remove the blood clot (which often resembles redcurrant jelly in appearance and texture). The source of bleeding will be found and stopped. The skull bone may or may not be replaced. Patients are then usually managed on intensive care. If the bone flap was removed they will require an artificial cranioplasty in due course to close the defect.
It is worth bearing in mind that the patient may still have issues with raised ICP, especially if there were other bleeds such as traumatic subarachnoid or contusions. They may require insertion of an external ventricular drain (EVD) or lumbar drain (LD) to divert CSF away and reduce ICP. This is in keeping with the Monro-Kellie doctrine detailed above.
Complications
Patients with an ASDH have a high mortality and can be left with permanent neurological deficits.
Patient who undergo decompressive surgery and/or are in intensive care are usually incredibly unwell even if they do not have many co-morbidities. Mortality is often high and patients can be left with neurological deficits such as weakness, paralysis or speech deficits especially if the injury happens on the dominant hemisphere (usually left).
They may develop systemic complications as a result of being on intensive care such as pneumonia (either aspiration or ventilator related), DVT/PE, urinary infections (catheter related) and so on. These patients have to be managed in a multidisciplinary fashion in conjunction with intensive care, neurosurgery, other specialities (as required), dietitians, physiotherapists and speech and language therapists.
Last updated: July 2021
Have comments about these notes? Leave us feedback
