Shingles
Notes
Overview
Shingles (herpes zoster) causes a characteristic vesicular rash that occurs due to reactivation of varicella-zoster virus (VZV).
Shingles is a viral infection caused by reactivation of varicella-zoster virus (VZV). The condition, also known as herpes zoster, causes a classic painful vesicular rash along the skin served by the single dermatome.
Primary VZV infection causes chickenpox, usually in children. Following resolution, the virus lays dormant in the dorsal root ganglia. In the advent of immunosuppression, the virus may reactivate leading to the classic vesicular rash along the skin served by the single dermatome.
Varicella-zoster virus
VZV is one of the human herpes viruses that is the cause of both chickenpox and shingles.
The human herpes viruses are a large family of DNA viruses that cause a range of infections in humans. VZV is also known as human herpes virus 3 (HHV-3).
VZV causes two distinct diseases depending on whether it is a primary VZV infection or reactivation:
- Primary VZV infection (chickenpox): characterised by a generalised pruritic vesicular rash, usually in children.
- Reactivation (shingles): characterised by a painful unilateral vesicular rash, restricted to a dermatomal distribution.
Shingles usually occurs due to alteration of the immune system. Age is the major factor in the development of shingles. This is because as we age, there is gradual deterioration in immune function known as immunosenescence. Any patient who is immunosuppressed for other reasons (e.g. systemic disease, cancer, post-transplantation) is at risk of shingles.
Risk factors
Age is the predominant risk factor for the development of shingles.
Any factor that suppresses the normal immune response can predispose to shingles.
- Age: up to 50% of patients who reach 85 years old will have experienced at least one episode of shingles
- Immunosuppression (e.g. chemotherapy, high dose steroids)
- Transplant recipients
- Autoimmune diseases: usually related to use of immunosuppressive medications
- HIV infection
- Other (e.g. co-morbid conditions such as CKD, COPD, diabetes)
Epidemiology
The lifetime risk of developing shingles is estimated at 20-30%.
Age is the major factor in developing shingles. The annual incidence in the UK is estimated at 1.85–3.9 cases per 1000 population. Up to 50% of patients who reach 85 years of age will have developed a single episode of shingles during their lifetime
Pathophysiology
The VZV lies dormant within the dorsal root ganglia.
Following a primary infection (i.e. chickenpox), VZV lies dormant with the dorsal root ganglia. When the immune system is weakened, it may extend out in a dermatomal distribution leading to the characteristic vesicular rash.
Patients with active lesions may transmit the virus to varicella naïve patients leading to development of chickenpox. Once the lesions are crusted over, they are considered non-infective.
Clinical features
Shingles classically causes a unilateral, erythematous, vesicular rash in a dermatomal distribution.
Shingles is characterised by a prodromal phase of paraesthesia and pain in the affected dermatome, which is followed by an erythematous maculopapular rash. This develops into clusters of vesicles (fluid-filled cysts), then pustules (pus-filled cysts), before bursting and crusting over.
The rash is unilateral and does not cross the bodies midline. Any dermatome may be affected including cranial nerves, but it most commonly occurs in the lumbar or thoracic dermatomes.
Signs and symptoms
- Paraesthesia
- Pain: throbbing, burning, stabbing (due to acute neuritis)
- Rash: erythematous maculopapular rash initially. Over several days groups of vesicles develop. Within 3-4 days these become pustular and then burst. By 7-10 days the lesions crust over in immunocompetent individuals.
- Scarring: hypopigmented or hyperpigmented areas can remain for months to years following an episode
- Systemic features (<20%): headache, fever, malaise, fatigue
- Hutchinson’s signs (see Herpes Zoster Ophthalmicus)
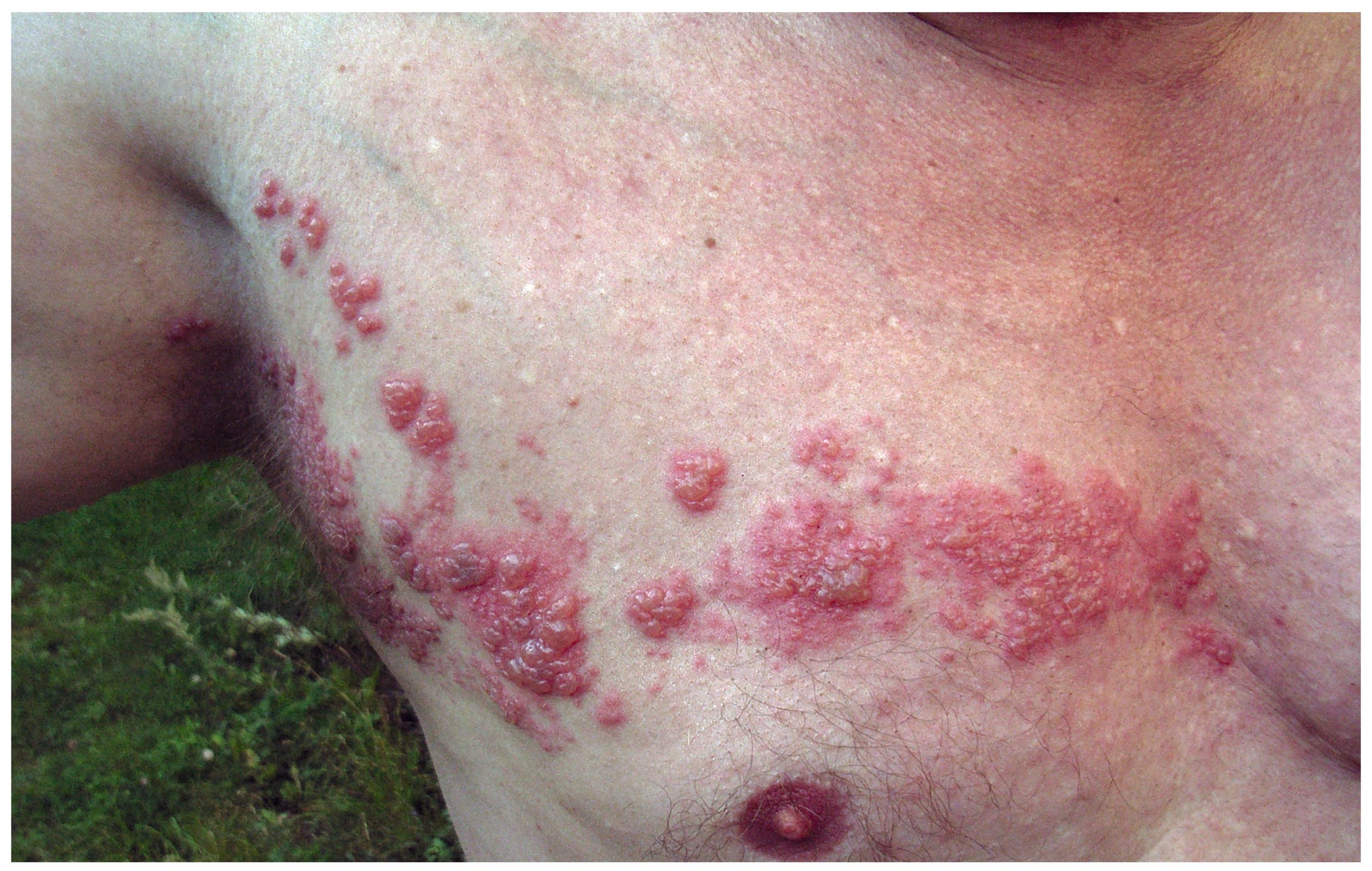
Class vesicular rash of shingles affecting the T3 dermatome.
Image courtesy of Fisle (Wikimedia commons)
Abnormal presentations
Patients who are older or immunosuppressed may have more atypical presentations.
- Absence of vesicular lesions (more likely if elderly)
- Prolonged rash: new lesions developing >7 days after presentations (usually in immunocompromised)
- Zoster sine herpete: describes pain without rash (rarely occurs)
- Disseminated disease: features of pneumonia, encephalitis, hepatitis (at risk if severely immunosuppressed)
- Multiple dermatomes
Herpes zoster ophthalmicus
This refers to reactivation of Herpes zoster within the distribution of the trigeminal nerve.
Reactivation of Herpes zoster within the trigeminal nerve (fifth cranial nerve) is known as herpes zoster ophthalmicus and can be sight-threatening due to involvement of the cornea.
An important sign of Herpes zoster ophthalmicus is Hutchinson’s sign. This describes the presence of vesicular lesions on the side or tip of the nose that represents the dermatome of the nasociliary nerve (branch of the Ophthalmic division of the trigeminal nerve). This sign correlates highly with subsequent eye involvement.
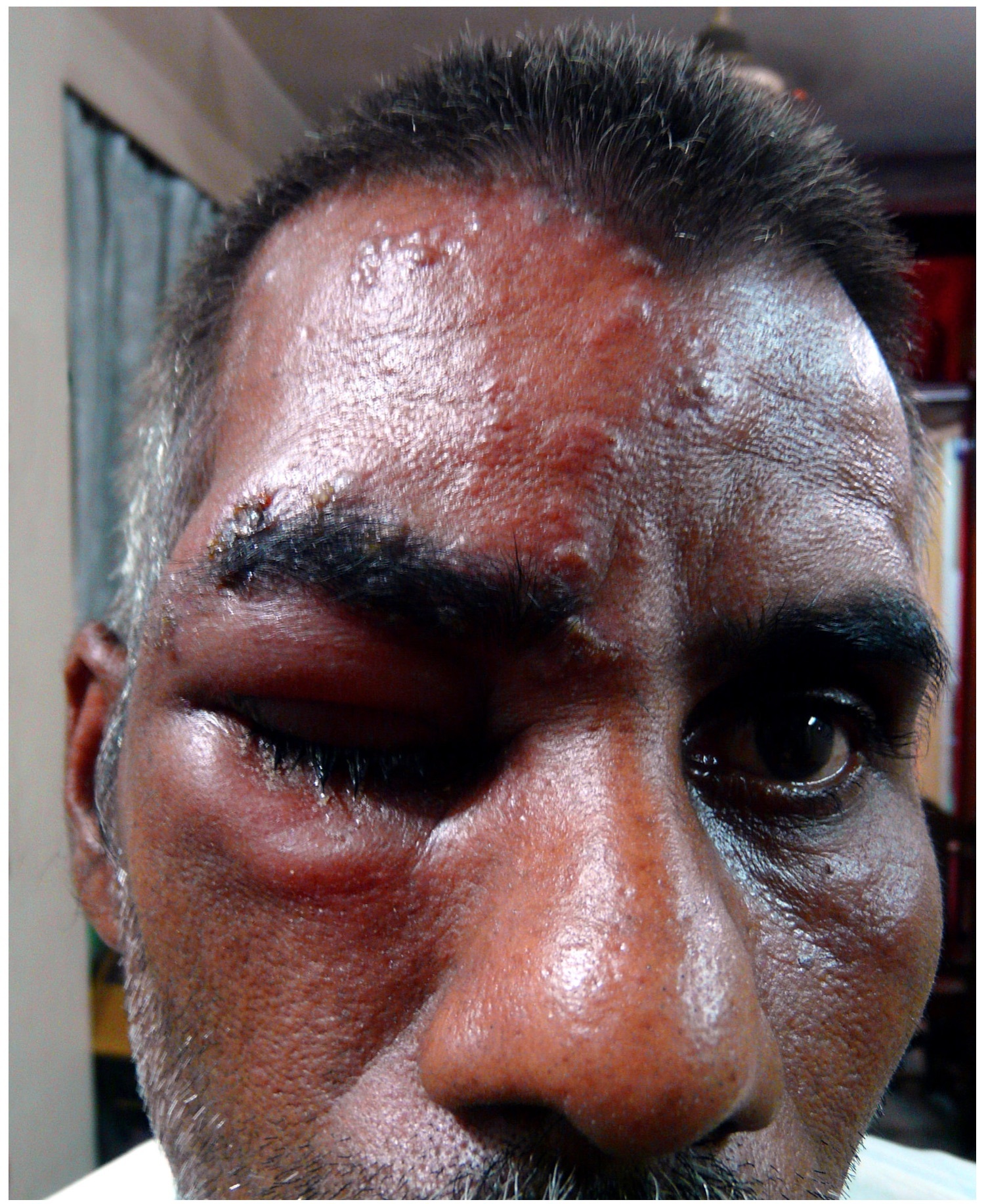
Herpes zoster ophthalmicus affecting the right eye
Image courtesy of Dr. Partha Sarathi Sahana (flickr)
Ramsay hunt syndrome
Ramsay hunt syndrome refers to the reactivation of herpes zoster in the geniculate ganglion of the facial nerve.
It is characterised by facial nerve palsy associated with a vesicular rash affecting the ipsilateral ear, hard palate and anterior two thirds of the tongue. For more information see Ramsay hunt syndrome notes.
Diagnosis & investigations
The diagnosis of shingles is usually a clinical diagnosis based on the appearance of the classical rash.
The diagnosis of shingles is based on the classic presentation of a painful, unilateral vesicular rash in a dermatomal distribution.
PCR testing
If the presentation is atypical or the diagnosis is unclear, VZV can be confirmed with polymerase chain reaction (PCR). A swab taken from a suspected lesion can be sent to the laboratory for PCR. This method can detect VZV DNA through amplification.
Testing for immunosuppression
Shingles often occurs in elderly or immunosuppressed individuals. The presence of shingles in an otherwise ‘healthy’ individual should prompt investigation for immunodeficiency (e.g. HIV testing, immunoglobulins, cancer assessment).
Management
Consider admission to hospital in patients with severe shingles, complications or significant immunosuppression.
The majority of patients with shingles can be managed with oral anti-viral therapy (e.g. aciclovir), which should be prescribed within 72 hours of rash onset.
Anti-viral therapy
Consider oral aciclovir, valaciclovir, or famciclovir for the treatment of shingles in the following groups:
- Immunocompromised (non-severely and not systemically unwell)
- Non-truncal involvement
- Moderate to severe pain or rash
- Patients >50 years old (reduces incidence of post-herpetic neuralgia)
- Pregnancy (seek specialist advice before initiating treatment)
If patients present >72 hours after rash onset, anti-viral therapy may be considered up to one week following rash onset. However, there is likely minimal benefit in immunocompetent individuals.
Analgesia
The choice of analgesia in patients with shingles depends on the severity of pain.
- Mild pain: offer simple analgesia (paracetamol with or without NSAIDs if no contraindication)
- Severe pain: offer simple analgesia (as per mild pain) plus consider neuropathic agents (e.g. amitriptyline, gabapentin).
A short course of steroids may be considered in patients with severe pain within the first two weeks of rash onset. This can only be considered in immuncompetent patients alongside anti-viral therapy.
If there is persistent pain following resolution of skin lesions, treat for post-herpetic neuralgia (see complications).
Hospital admission
Patients may require inpatient admission for intravenous antiviral therapy and monitoring, or management of complications, in the following groups:
- Severe complications (e.g. meningitis, encephalitis)
- Herpes zoster ophthalmicus
- Severely immunocompromised
- Severe infection (e.g. severe rash, widespread, or systemic features)
- Immunocompromised child
Basic advice
Patients remain infectious until all lesions have crusted over, which usually occurs at 5-7 days. It is important to avoid contact with the following groups:
- People who have not had chickenpox
- Immunocompromised individuals
- Babies <1 month
Good hygiene advise including avoiding sharing clothes, hand hygiene and avoiding work, school or day care (if lesions are weeping) is important.
Post-exposure prophylaxis
Varicella zoster immunoglobin refers to a scarce product of pooled antibodies against VZV. It may be offered to VZV antibody negative pregnant woman (≤ 20+0 weeks) who have had significant exposure to chickenpox or shingles. It may also be offered for severe neonatal infections.
Vaccination
A shingles vaccination may be offered to patients aged 70 years old if there are no contraindications. It is a live attenuated vaccine (Zostavax®) that cannot be administered to pregnant woman or certain immunosuppressed groups due to risk of disseminated infection.
The vaccine is effective at reducing the incidence and severity of shingles including post-herpetic neuralgia.
Complications
A number of serious complications may develop secondary to shingles.
Complications associated with shingles may range from mild to severe depending on age, co-morbidities and underlying immunocompetence.
- Scarring: hypo- or hyperpigmented areas
- Post-herpetic neuralgia (see below)
- Secondary bacterial infection
- Ramsay hunt syndrome
- Herpes zoster ophthalmicus
- Motor neuropathy
- CNS involvement: encephalitis, meningitis, myelitis
- Disseminated infection
Post-herpetic neuralgia
This is the most common complication associated with shingles and describes pain that is persistent, or appears more than, 90 days after the rash onset.
Post-herpetic neuralgia is due to neuritis and nerve damage in the affected region. Post-herpetic neuralgia is more common in older patients and rare in patients <50 years old.
Treatment options include:
- Conservative: wearing loose clothes, consider protecting sensitive areas and applying cold packs
- Mild to moderate pain: simple analgesia (paracetamol with or without codeine) or topical treatments (e.g. capsacin cream or lidocaine plaster)
- Uncontrolled with simple analgesia: consider neuropathic agents (e.g. amitriptyline, duloxetine, gabapentin, or pregabalin)
Last updated: July 2021
Have comments about these notes? Leave us feedback
