Chickenpox
Notes
Overview
Chickenpox is a highly contagious viral illness that causes a classic vesicular rash.
Chickenpox is predominantly an illness of childhood that is caused by the varicella-zoster virus (VZV). It causes a highly contagious vesicular rash that is managed symptomatically in the majority of cases.
In children, chickenpox is most commonly a benign self-limiting illness. However, in adults or those immunosuppressed, it can cause a severe illness with severe complications (e.g. varicella pneumonia).
Varicella-zoster virus
VZV is one of the human herpes viruses that is the cause of both chickenpox and shingles.
The human herpes viruses are a large family of DNA viruses that cause a range of infections in humans. VZV is also known as human herpes virus 3 (HHV-3).
VZV causes two distinct diseases depending on whether it is a primary VZV infection or reactivation:
- Primary VZV infection (chickenpox): characterised by a generalised pruritic vesicular rash, usually in children.
- Reactivation (shingles): characterised by a painful unilateral vesicular rash, restricted to a dermatomal distribution.
Epidemiology
The peak incidence of chickenpox occurs in children < 10 years old.
By 15 years old, it is estimated that >90% of young people have experienced chickenpox. The peak incidence of the disease occurs between March-May.
Pathophysiology
Following recovery from chickenpox, the virus lies dormant within the dorsal root ganglia.
VZV is a highly contagious virus that is spread by direct contact with vesicle fluid from skin lesions or respiratory droplets from nasopharyngeal secretions.
Following transmission, the incubation period is around 14-16 days (period from acquisition of the virus to symptom onset). Patients then develop the characteristic generalised papular rash that becomes vesicular. Patients are considered infective 48 hours before rash onset until the typical skin lesions have fully crusted over.
The majority of patients make a complete recovery without intervention. The immune system is unable to completely clear the virus, which remains dormant within the dorsal root ganglia of nerves. As we age, or through immunosuppression, the virus may replicate and reemerge as shingles. For more information see Shingles notes.
Clinical features
Chickenpox causes a classic generalised vesicular rash.
Chickenpox usually develops within 15 days of exposure to the virus, which starts with a prodromal illness of fever and malaise followed by a generalised vesicular rash within 24 hours.
Signs and symptoms
- Fever
- Malaise
- Feeding problems
- Vomiting/diarrhoea
- Headache
- Rash
Rash
The rash starts as small erythematous macules on the scalp, face, trunk and proximal limbs. This progress to papules and then develops into intensely pruritic vesicles (fluid-filled cysts) before becoming pustules (pus-filled cysts). They can affect any area including palms, soles, mucous membranes and genitalia. The pustules then burst and begin to crust over from around 5 days after rash onset. There is often temporary hypopigmentation of these skin areas after the crusting has fallen off over 1-2 weeks.
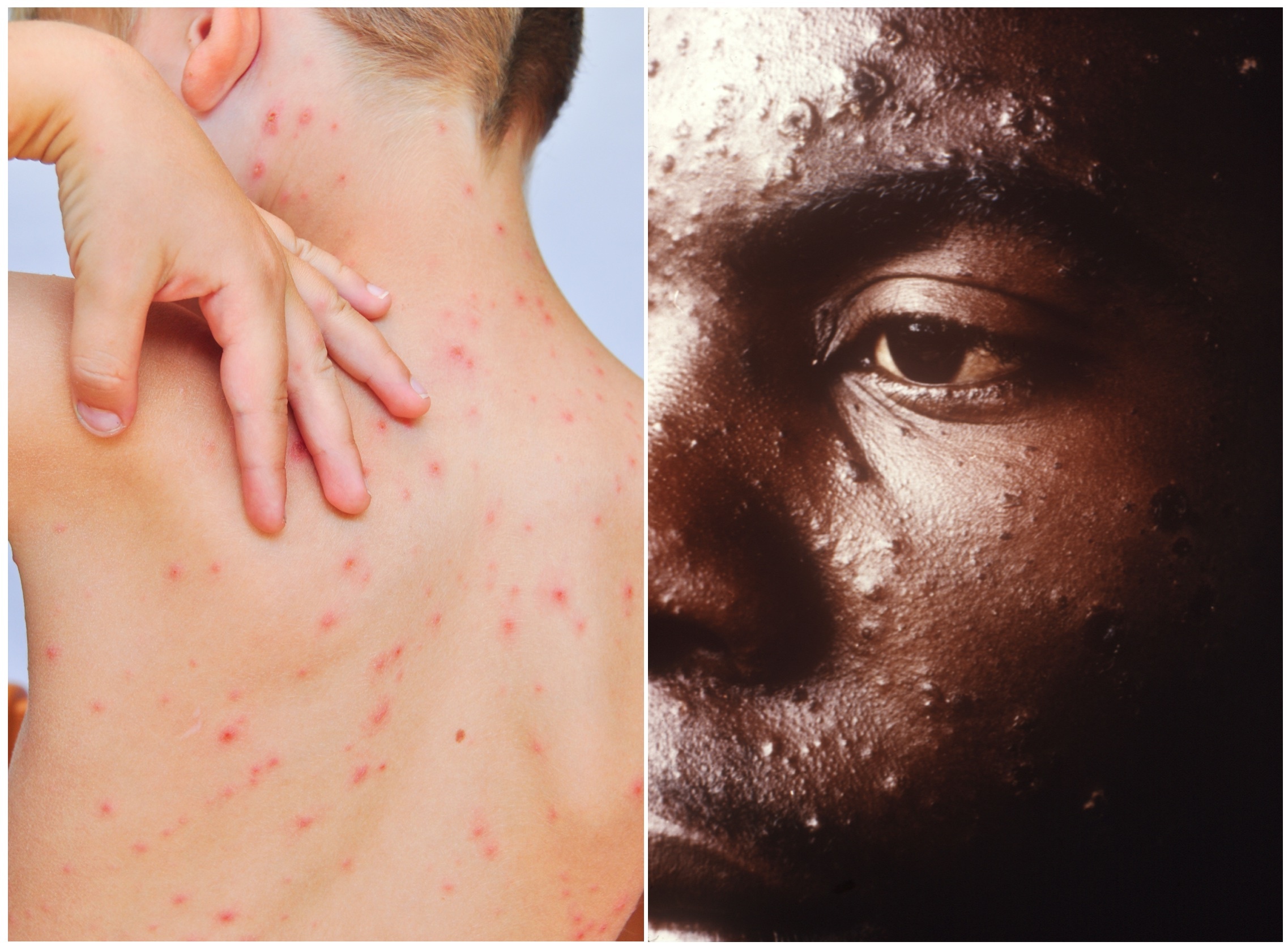
Typical rash of chickenpox
Diagnosis & investigations
The diagnosis of chickenpox is usually made clinically by the presence of the characteristic vesicular rash.
Chickenpox is a clinical diagnosis based on the presence of the typical vesicular rash in children. In older children and adults, the presentation may be atypical or more widespread. VZV antibodies can be checked to assess for previous exposure to the virus if there is any uncertainty. A formal diagnosis can be made from skin swabs of infected lesions for viral polymerase chain reaction (PCR). This is a laboratory method of amplifying viral DNA.
Management
In the majority of cases, chickenpox is self-limiting and the management supportive.
Most cases of chickenpox can be managed symptomatically with paracetamol, but NSAIDs (e.g. ibuprofen) should be avoided. Calamine lotion can be used to help with pruritus and anti-histamines (e.g. Chlorphenamine) may be used in children >1 year old.
It is important to maintain adequate hydration and children should remain away from school or nursery until all vesicles have crusted over. It is critical to avoid high risk groups as there is risk of serious infection. These include:
- Infants ≤ 4 weeks old
- Immunocompromised patients
- Pregnant woman
Anti-viral therapy (e.g. aciclovir) is generally only recommended in adults and older children (>14 years old) who present with chickenpox within 24 hours of rash onset.
Pregnancy
Chickenpox in pregnancy can be severe with risk to both mother and fetus.
Chickenpox in pregnancy can be severe with up to 10% developing varicella pneumonia. Those with severe chickenpox require admission to hospital. If admission is not required, specialist advice should be sought and anti-viral therapy can be considered.
Pregnant woman should avoid contact with patients with chickenpox. If exposed, VZV antibody status (IgG) should be checked and varicella zoster immunoglobulin (VZIG) considered if < 20 weeks gestation and negative antibodies.
Fetal varicella syndrome
If pregnant mothers are infected with VZV in the first 28 weeks of pregnancy then the fetus is at risk of fetal varicella syndrome.
Fetal varicella syndrome is an intrauterine infection characterised by one or more of the following:
- Skin scarring
- Hypoplasia of limbs
- Neurological disorders: microcephaly (small head), learning difficulties, bladder/bowel dysfunction
- Eye disorder: microphthalmia (small eyes), chorioretinitis, cataracts
This syndrome occurs in <1% in the first trimester and 2% between 13-20 weeks gestation.
Complications
Development of erythema and pain around lesions with associated high fever is suspicion of superadded bacterial infection.
The majority of children will have a benign self-limiting illness. Complications are more often seen in neonates, adults and those immunosuppressed when the disease can be more widespread and lead to organ damage. Possible complications:
- Superadded bacterial infection
- Dehydration
- Pneumonia
- CNS involvement: Encephalitis, meningitis, myelitis, Reye’s syndrome
- Dissemination: characterised by pneumonia, hepatitis, encephalitis and disseminated intravascular coagulation (DIC).
- Haemorrhagic varicella
NOTE: Reye’s syndrome is a rare syndrome most commonly seen in children in association with aspirin use or following a viral infection (chickepox, influenza). It is characterised by encephalopathy and liver impairment. It is thought that inborn errors of metabolism may predispose to, or are responsible for, Reye's syndrome.
Last updated: July 2021
Have comments about these notes? Leave us feedback
