Anogenital herpes
Notes
Overview
Anogenital herpes is caused by herpes simplex virus 1 & 2 and leads to painful ulcerated genital lesions.
Anogenital herpes is characterised by multiple, painful, ulcerated genital lesions. They arise as small vesicles that progress to pustules, which subsequently ulcerate and crust over.
Anogenital herpes can be caused by herpes simplex virus 1 (HSV1) or herpes simplex virus 2 (HSV2), which are both part of the larger family of human herpesviruses (HHVs). This family also includes varicella-zoster virus, Epstein-Barr virus and cytomegalovirus.
Epidemiology
Worldwide there are over 23 million cases of HSV infection per year.
HSV-1 is usually acquired in childhood and often causes oral mucosal lesions. It is estimated that up to 67% of patients aged 0-49 years old have serological evidence of prior infection (i.e. developed antibodies). Worldwide, the prevalence of HSV-2 infection among patients 15-49 years old is estimated at 11%.
Worldwide HSV-2 is the most common cause of anogenital ulcers, but in the UK HSV-1 is now the most commonly implicated. The prevalence of both HSV-1 and HSV-2 is higher in women than men.
Aetiology
Anogenital herpes are most commonly due to HSV-1 in the UK.
Herpes simplex virus
Anogenital herpes is caused by HSV-1 and HSV-2
- HSV-1: causes both oro-labial herpes and genital herpes (most common cause in UK).
- HSV-2: causes genital herpes. More likely to cause recurrent herpes.
Terminology
- Primary infection: first anogenital herpes infection. No serological evidence of previous infection (i.e. negative antibodies).
- Non-primary infection: first anogenital herpes infection. Serological evidence of previous infection (i.e. positive antibodies).
- Recurrent infection: recurrent, clinically symptomatic, anogenital herpes. Due to reactivation of HSV-1/HSV-2.
Transmission
Anogenital herpes is transmitted by direct contact with infected secretions, which commonly occurs during sexual intercourse. Humans are the only hosts involved in infection.
The majority of infections are acquired subclinically, which means patients do not develop symptoms. This is in part due to asymptomatic viral shedding. In patients with HSV-2 infection, only one-third of patients are symptomatic at the time the virus is acquired. If symptoms do develop, they usually occur within 2-14 days of acquisition.
Recurrent infection
Patients are at risk of recurrent infection because the virus enters a dormant ‘latent phase’ within the cell ganglia of nerves. A variety of triggering events (e.g. fever, immunosuppression, menstruation) can lead to reactivation with symptomatic anogenital lesions or covert viral shedding.
Patients with HSV-2 infection are more likely to develop recurrent, clinically symptomatic, anogenital herpes. It is estimated to be four times more frequent compared to HSV-1. Recurrence declines over time, although the clinical course is variable.
Pathophysiology
After the initial infection, HSV is able to enter a dormant latent phase within nerve cell ganglia.
HSV is unique in that it has the ability to invade and remain dormant within nerves. After contact with infected secretions, the virus replicates within the epidermis before infecting sensory or autonomic nerve ganglia. Here, it causes a lifelong infection by evasion of the immune system and enters a latent phase.
There are typical locations of HSV in both oro-labial and anogenital herpes:
- Oro-labial herpes: trigeminal ganglia
- Anogenital herpes: sacral nerve root ganglia
Several triggering events can lead to reactivation that may result in a clinically symptomatic infection (i.e. development of painful ulcerated lesions) or an asymptomatic infection with viral shedding. It is able to travel down nerve axons to reach mucosal and cutaneous surfaces. Patients who are immunocompromised are at a higher risk of reactivation, which may be more severe.
Clinical features
Anogenital herpes is characterised by multiple, painful ulcers and tender lymphadenopathy.
Site of lesions
- Men / transwomen: glans penis, foreskin (prepuce), penile shaft and less commonly scrotum, thigh and buttocks. Rectal and perianal lesions seen in men who have sex with men (MSM).
- Women / transmen: Vulva, labia, vaginal vestibule and introitus. The vaginal mucosa is usually inflamed and cervical involvement is seen in 70-90%
Symptoms
- Asymptomatic
- Painful vesicle, pustule or ulceration: usually multiple lesions of different ages
- Vaginal/urethral discharge
- Dysuria
- Systemic symptoms: fever, headache, malaise, myalgia (more common in primary infection)
- Proctitis: bleeding, tenesmus, pain, discharge (more common in MSM)
Signs
- Vesicles
- Pustules
- Ulceration: usually evidence of crusting over
- Lymphadenopathy/lymphadenitis (inguinal): usually tender and bilateral. Seen in around 30%. Unilateral more common in recurrent infection
- Urinary retention: if pelvic autonomic nerves affected
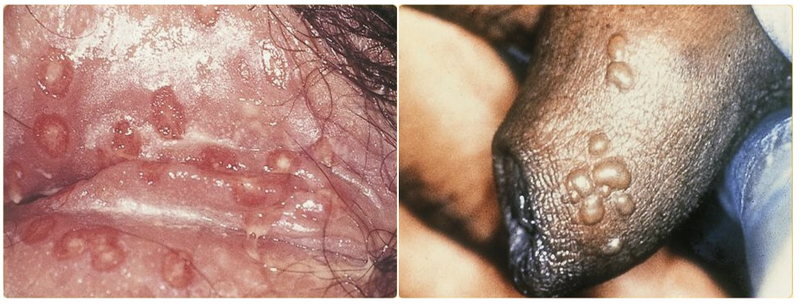
Typical anogenital herpetic lesions located on the vulva (left) and penis (right)
Images courtesy of SOA-AIDS Amsterdam
Complications
- Superinfection: lesions may become infected by bacteria (e.g. streptococcal spp.) or fungi (e.g. candida spp.)
- Autonomic neuropathy: can cause urinary retention
- Autoinoculation: lesions can be passed to other areas of skin through direct contact (e.g. fingers, adjacent skin)
- Central nervous system: aseptic meningitis and encephalitis. More likely in patients with HIV co-infection or marked immunosuppression.
- Other: hepatitis, oesophagitis and keratitis among others.
Diagnosis & investigations
The diagnosis of anogenital herpes should be made by identification of HSV within infected lesions.
NAATs
Nucleic acid amplification tests (NAATs) using polymerase chain reaction (PCR) are the test of choice for the diagnosis of anogenital herpes. This test is performed on swabs taken from suspected lesions. It is important to take rectal swabs for HSV in MSM or in patients with symptoms of proctitis.
Serum DNA levels of HSV can be completed, but usually reserved in patients who are immunosuppressed or develop complications.
Culture
Viral culture for HSV can be completed but it is less effective compared to NAATs, especially in patients with late or mild recurrent symptoms.
Serology
Testing blood samples for an antibody response can be completed in patients with suspected anogenital herpes. A serum IgG response agents HSV-1 or HSV-2 suggest infection at some point, but is unable to inform on a current infection. Serum IgM that implies recent infection is not reliable for HSV-1/2 infections.
HSV-2 antibodies indicate anogenital herpes. HSV-1 antibodies indicate oro-labial or anogenital herpes but cannot differentiate between them.
Serology is helpful for:
- Recurrent genital ulcers (unknown cause)
- To aid counselling
- Investigating asymptomatic partners of patients with anogenital herpes
Other investigations
In patients with suspected anogenital herpes, it is important to refer for assessment at a genitourinary medicine (GUM) clinic so that a full sexual health screen can be completed including testing for other STIs like chlamydia, gonorrhea, syphilis and HIV.
Testing for other causes of genital ulceration (e.g. Lymphogranuloma venereum, chancroid, granuloma inguinale) can be considered if HSV testing is negative.
Management
Anti-viral therapy with aciclovir forms the backbone of treatment in anogenital herpes.
Conservative therapy
Anogenital herpes can be distressing and painful, particularly the first episode. Basic advice regarding saline bathing (washing with simple mixture of salt and water) and analgesia including topical anaesthetic agents (e.g. lidocaine) should be offered to all patients.
Pharmacological therapy
Anti-viral therapy should be offered to patients who present within 5 days of symptom onset, if new lesions are still appearing or systemic symptoms are ongoing. Treatment reduces the duration and severity of illness but does not alter the natural history or chance of recurrent infections.
Oral treatment is more effective than topical. Combination therapy (oral and topical) confers no additional benefit.
Options include:
- Aciclovir 400 mg three times a day for 5 days, OR
- Aciclovir 200 mg five times a day for 5 days, OR
- Valaciclovir 500 mg twice daily for 5 days
Recurrent infections
Those with recurrent infections usually have minor symptoms and episodes are self-limiting. There are different options for treating recurrent infections, which include:
- Supportive care only
- Episodic antivirals: can be started by patients themselves at onset of symptoms
- Short-course options: Aciclovir 800 mg three times daily for 2 days or Valaciclovir 500 mg twice daily for 3 days
- Five day course options: same treatment for first infection (see above)
- Suppressive therapy: offered to patients with ≥ 6 episodes/year or those where it is causing major psychological distress
- Aciclovir 400 mg twice daily, OR
- Valaciclovir 500 mg once daily
Patients with breakthrough infections on suppressive therapy can increase their medication to treatment dose until the infection resolves.
Prevent transmission
It is important to give patients with anogenital herpes the following advice to prevent transmission:
- Abstinence: do not have sexual contact during infection or prodrome (symptoms prior to development of lesions)
- Asymptomatic transmission: HSV can still be transmitted without lesions (due to asymptomatic viral shedding)
- Role of condoms: Male condoms reduce transmission when correctly applied (do not completely remove risk)
- Suppressive therapy: this reduces a partners risk of acquiring symptomatic anogenital herpes
- Disclosure: it is advised patients disclose their diagnosis in all relationships. Disclosure is associated with lower transmission risk and protects against legal action.
Discussion about disclosure and transmission should always be documented.
Co-infection with HIV
Anogenital herpes may be severe and prolonged in patients who are co-infected with HIV. This is particularly concerning in patients with a severe degree of immunosuppression. It can lead to life-threatening complications (see chapter on complications) if not treated.
The dose and duration of anti-viral therapy is higher in patients co-infected with HIV.
- Aciclovir 400 mg five times a day for 7-10 days, OR
- Valaciclovir 500-1000 mg twice daily for 10 days
A specialist in HIV medicine should be consulted when managing patients co-infected.
Complications
Complications from HSV are more likely to occur in patients who are immunosuppressed (e.g. HIV co-infection).
Patients with complications often require hospital admission for intravenous therapy.
- Aseptic meningitis
- Encephalitis
- Pneumonia
- Oesophagitis
- Hepatitis
- Urinary retention
Last updated: March 2021
Further reading
British Association for Sexual Health and HIV (BASHH) guidelines.
Have comments about these notes? Leave us feedback