Chancroid
Notes
Overview
Chancroid is a sexually transmitted infection caused by Haemophilus ducreyi.
Chancroid is a sexually transmitted infection (STI) caused by the organism Haemophilus ducreyi. It is highly contagious and characterised by multiple, deep painful ulcers. It is one of the sexually transmitted causes of genital ulcers.
Traditionally, chancroid was very common, but with more attention paid to STI transmission with the rise in HIV cases in the 1980’s, the prevalence of chancroid has been falling. Herpes simplex is now the most common genital ulcerative disease.
Genital ulcers
The major causes of genital ulcers include:
- Syphilis: characterised by a single painless ulcer (chancre)
- Herpes simplex virus (HSV): multiple painful vesicles that ulcerate
- Granuloma inguinale: one or more nodules that eventually ulcerate. Usually painless
- Lymphogranuloma venereum (LGV): one or more painless papules that develop into shallow ulcers
- Chancroid: multiple deep painful ulcers with a purulent base.
Epidemiology
Chancroid is rarely observed within the UK.
There are few cases of chancroid annually within the UK. These are usually acquired abroad from high prevalent areas. Chancroid is still prevalent in parts of Africa (e.g. Zambia, Mozambique), the Caribbean basin and Southwest Asia.
The disease is most commonly seen in young (21-30 years old), sexually active patients with the highest incidence in young non-white and uncircumcised males.
Aetiology & pathophysiology
Chancroid causes ulcerative genital lesions secondary to the bacterium Haemophilus ducreyi.
Chancroid is caused by the bacterium Haemophilus ducreyi, which is a gram negative bacilli and highly infective. The incubation period (time between infection and develop of symptoms) is usually 4-7 days.
It is transmitted through direct contact with infected lesions during sexual intercourse. The bacterium is able to establish infection by penetrating through breaks in the skin or mucous membranes. Once barriers are breached, it causes a local inflammatory response with early development of painful papules. These deteriorate into deep, painful ulcers due to a number of virulence factors that cause necrosis of surrounding cells.
Due to local tissue inflammation and destruction, chancroid disrupts the normal integrity of the skin barrier and increases the risk of HIV transmission.
Clinical features
Chancroid is characterised by multiple, deep painful ulcers and lymphadenitis.
Sites
- Men/transwomen: foreskin (prepuce), coronal sulcus of glans penis, glans penis and frenulum.
- Women/transmen: labia minora and fourchette.
- All: extragenital lesions rare (e.g. fingers, breasts).
Features
- Painful papules: early lesion that deteriorates into pustule then ulcer. May be one or more lesions
- Ulcers: typically deep, painful and purulent with a ragged edge. Easily bleed when touched
- Lymphadenopathy: usually painful and unilateral in the inguinal region. Seen in 50% of men, less often in women. Usually develop 1-2 weeks following infection.
- Buboe: infected, painful lymphadenitis that ulcerates and becomes suppurative. Can cause chronic draining sinuses.
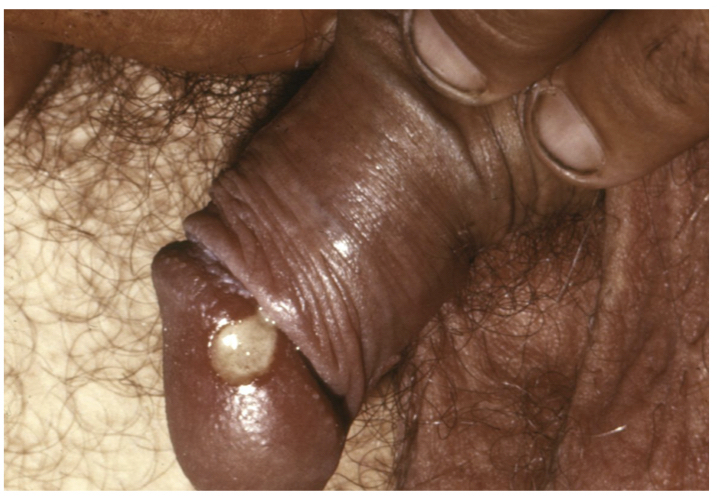
Typical ulcer of chancroid on corona of glans penis. Image courtesy of CDC.
Uncommon lesions
- Transient chancroid: short period of genital ulcers following by lymphadenitis
- Dwarf chancroid: similar appearance to herpes simplex without lymphadenopathy
- Giant chancroid: multiple small lesions coalesce to form giant lesion
- Follicular chancroid: pyogenic infection (i.e. producing excess PUS)
Diagnosis & investigations
Traditionally, microscopy & culture is needed to diagnose chancroid but sensitivity is <80%.
There are limited investigations that can be used to diagnosis chancroid.
Diagnostic tests
- Nucleic acid amplification tests (NAATs): used to detect genetic material of H. ducreyi. Better sensitivity that microscopy and culture, but no commercial assays available.
- Microscopy: swabs taken from ulcer base. On gram stain, may show characteristic gram negative coccobacili, but sensitivity only 50%.
- Culture: swabs taken from ulcer base. Fastidious organism, so difficult to culture with sensitivity in prevalent areas estimated at 60-80%.
- Serology: assesses for antibodies that have been generated against H. ducreyi. Difficult to differentiate between past and recent infection. Combined with other tests (e.g. syphilis screening and HSV testing) to come to probable diagnosis.
Differential diagnosis
Chancroid presents very similarly to other ulcerative genital lesions including granuloma inguinale, LGV and herpes simplex. It can be difficult to distinguish between these conditions, particularly granuloma inguinale.
Other investigations
Patients with suspected Chancroid require referral and assessment at a genitourinary medicine (GUM) clinic. This enables a full sexual health screen including testing for other STIs such as chlamydia, gonorrhoea, syphilis and HIV.
Management
A single dose of azithromycin is an effective first line treatment for chancroid.
General advice
All patients with chancroid should be advised to avoid sexual contact until treatment with antibiotics is completed and they have undergone appropriate follow-up. All sexual contacts should have contact tracing as advised by the GUM clinic. This usually refers to all sexual partners within 10 days prior to the onset of symptoms.
Pharmacological management
Single dose treatment with azithromycin should be avoided in patients who are co-infected with HIV. In these cases ciprofloxacin or erythromycin is usually preferred.
- Single dose options:
- Azithromycin 1 g orally as a single dose, OR
- Ceftriaxone 500 mg intramuscularly as a single dose, OR
- Multi-dose options:
- Ciprofloxacin 500 mg orally twice daily for three days, OR
- Erythromycin 500 mg orally four times a day for seven days
Complications
Complications from chancroid are most commonly seen in men.
- Phimosis: narrowing of the opening of the foreskin
- Increase risk of HIV transmission
- Local fibrotic reaction of healed ulcers
Last updated: March 2021
Further reading
British Association for Sexual Health and HIV (BASHH) guidelines.
Have comments about these notes? Leave us feedback
