Angio-oedema
Notes
Overview
Angio-oedema refers to a self-limiting, localised swelling that affects the skin or mucosal tissue.
Angio-oedema is a common condition that refers to localised swelling within the skin or mucosal tissue. It commonly occurs in non-gravitational areas such as the face, lips, mouth, throat or larynx. It typically occurs within minutes to hours and spontaneously resolves within 24-48 hours. It is due to extravasation of fluid within the subcutaneous or submucosal tissue due to disruption of vascular integrity.
Angio-oedema may occur with or without urticaria and can be part of a more systemic anaphylactic reaction. Angio-oedema can be life-threatening if it is part of anaphylaxis or swelling in the larynx, upper airway, or tongue is so severe it leads to airway obstruction.
Epidemiology
Angio-oedema is a common condition seen in all ages.
Angio-oedema is common and often occurs with urticaria. Approximately 10% of patients will experience angio-oedema without urticaria, which is often drug-induced or related to inherited C1 inhibitor deficiency (i.e. hereditary angio-oedema). However, hereditary angio-oedema is rare (1 in 10,000-50,000).
Pathophysiology
The hallmark of angio-oedema is vasodilatation and swelling in the subcutaneous and submucosal tissue.
Angio-oedema results from vasodilatation and extravasation of fluid into the deep dermis, subcutaneous tissue and/or submucosa. It characteristically occurs in non-gravitational dependent areas (e.g. face, lips, larynx, bowel). Angio-oedema may result from the release of inflammatory mediators by mast cells similar to urticaria that can be IgE or non-IgE-mediated. Alternatively, angio-oedema results from release of bradykinin that also affects vascular permeability. Bradykinin-mediated angioedema is not associated with urticaria and/or pruritus.
Urticaria is due to release of inflammatory mediators by mast cells and basophils in the upper dermis. Both immune (e.g. IgE-mediated/non-IgE-mediated) and non-immune mechanisms can lead to the release of these inflammatory mediators including histamine and cytokines. These cause vasodilatation in the skin leading to localised swelling and marked itching.
Aetiology
Angio-oedema is broadly divided into three aetiological mechanisms: mast-cell mediated, bradykinin-mediated and idiopathic.
The causes of angio-oedema can be broadly placed into three groups based on the underlying aetiological mechanism:
- Mast cell-mediated
- Bradykinin-mediated
- Idiopathic
Mast cell-mediated
Refers to the activation of mast cells and release of chemical mediators such as histamine. Causes can be due to IgE-mediated mechanisms (i.e. allergic reactions), direct mast cell activation or disruption of arachidonic acid metabolism. Mast-mediated angio-oedema almost always occurs with urticaria and/or pruritus.
- Allergic reactions: food, drugs, latex, insect bites/stings, food additives
- Non-allergic reaction (direct mast cell activation): radiological contrast agents, certain foods, certain medications (e.g. opiates).
- NSAIDs and aspirin: rarely cause an IgE-mediated allergy. More commonly due to inhibition of cyclooxygenase 1 (COX-1) as part of arachidonic acid metabolism. Results in a non-immunological mediated ‘pseudoallergy’ that can occur with urticaria.
Bradykinin-mediated
In bradykinin-mediated angio-oedema there is an increased generation of bradykinin or inhibition of bradykinin degradation. Kininogen is usually converted to bradykinin by kallikrein. Bradykinin causes vessel vasodilatation via release of chemical mediators such as prostacyclin and nitric oxide. This increases vascular permeability and leads to swelling. Angiotensin converting enzyme (ACE) promotes bradykinin degradation.
This type of angio-oedema is not associated with urticaria and/or pruritus and the management of the condition is different to mast cell-mediated disorders. There are three broad causes of bradykinin-mediated angio-oedema:
- Medications: ACE inhibitors most commonly implicated. Others include dipeptidyl peptidase-4 (DPP-4) inhibitors, fibrinolytic agents (e.g. alteplase), statins and proton pump inhibitors
- Hereditary angio-oedema: a collection of inherited autosomal dominant disorders due to abnormalities in the level or function of the complement protein C1 inhibitor (previously known as C1 esterase). Rarely hereditary angio-oedema with normal C1 inhibitor may be seen with genetic mutations in other genes. Discussed further below
- Acquired angio-oedema due to C1 inhibitor deficiency: usually occurs in older patients and associated with an underlying lymphoproliferative disorder
Idiopathic
When the underlying cause of angioedema cannot be identified it is referred to as ‘idiopathic angio-oedema’. Idiopathic angio-oedema is broadly divided into histaminergic or non-histaminergic.
- Histaminergic: closely linked to chronic spontaneous or inducible urticaria that occurs with or without angio-oedema
- Non-histaminergic: occurs in the absence of urticaria and may reflect rare subtypes of hereditary angio-oedema
A number of additional causes of angio-oedema are recognised (e.g. infections, herbal medicines, disorders with eosinophilia) of which the underlying mechanism is unknown.
Hereditary angio-oedema
A group of autosomal dominant inherited disorders that result in recurrent, self-limiting angio-oedema.
Hereditary angio-oedema (HAE), previously known as C1 esterase deficiency, is an autosomal dominant disorder that results in recurrent attacks of angio-oedema without urticaria and/or pruritus. The condition usually presents in childhood or early adolescence with recurrent angio-oedema and abdominal pain due to involvement of the bowel wall. Attacks may be mild and self-limiting or severe and life-threatening due to extensive upper airway oedema. May be precipitated by trauma, infection, stress or many other factors.
HAE is typically due to abnormalities in the level or function of the complement protein C1 inhibitor, although there are different forms of the inherited condition:
- HAE type I (85%): reduced levels of C1 inhibitor. Plasma protein level and function are low
- HAE type II (15%): normal or elevated levels of C1 inhibitor but function is low when tested
- HAE type III (rare): normal C1 inhibitor level and function. Specific mutations identified in genes of different proteins (e.g. Coagulation factor XII, plasminogen)
The diagnosis should be suspected in patients with recurrent angio-oedema without urticaria that usually lasts 2-5 days without treatment. In addition, symptoms are usually poorly responsive to treatment (e.g. anti-histamines). These patients should undergo complement testing to confirm the diagnosis.
A shorter duration of symptoms (< 24 hours) or presence of urticaria makes the diagnosis much less likely.
Clinical features
Angio-oedema is characterised by localised swelling in subcutaneous or submucosa tissue (e.g. face, lips, larynx).
Angio-oedema may occur with or without urticaria and features of anaphylaxis. This depends on the underlying cause of angio-oedema. Urticaria refers to a red, raised, itchy rash that can be quite widespread. For more information see urticaria notes.
The features of angio-oedema are dependent on the site involved. Swelling commonly affects loose connective tissue in non-gravitational areas (e.g. face, lips, mouth, throat, uvula, larynx, genitalia). There are characteristic features that help to differentiate angio-oedema from other forms of oedema:
- Onset within minutes to hours
- Spontaneous resolution within hours to days
- Asymmetrical
- Involvement of typical areas (e.g. face, lips, throat)
- Other features of allergy present
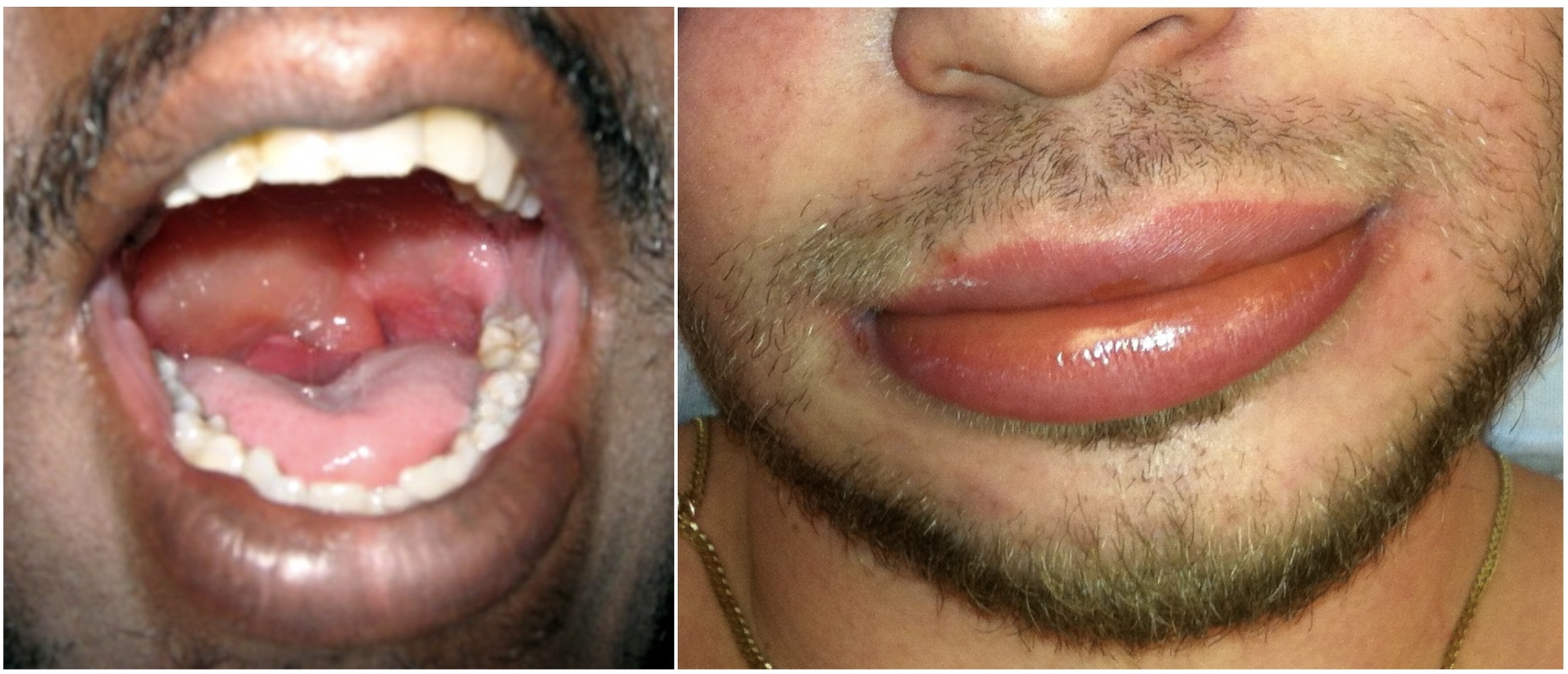
Examples of angio-oedema (left throat, right lips)
Images courtesy of Grook Da Oger (left) and James Heilman (Right). Wikimedia commons.
Larynx
- Hoarse voice
- Throat tightness
- Oropharyngeal dysphagia
- Airway compromise and stridor
Lips and mouth
- Swollen lips, tongue, uvula
- Airway compromise and stertor
Skin and mucous membranes
- Diffuse, non-pitting and tense swelling
- Non-pruritic unless associated with urticaria
- Absent or mild pain
- Usually resolves without a residual mark
Bowel
- Nausea/vomiting
- Diarrhoea
- Colicky abdominal pain
Diagnosis & investigations
The diagnosis of angio-oedema is made clinically based on the history and typical skin/mucosal swelling.
A definitive diagnosis angio-oedema is made by direct visualisation of typical subcutaneous/submucosal swelling, which affects classical areas (e.g. lips, face, mouth). The swelling will occur within minutes to hours and resolve over hours to days.
Critically, in patients presenting with angio-oedema that is affecting the airway or with features of a generalised allergic reaction (e.g. chest tightness, shortness of breath, throat tightness, nausea, vomiting, abdominal pain, lightheadedness, etc) then urgent management and airway protection is vital before a full comprehensive diagnostic assessment.
The underlying aetiology may be apparent from the history (e.g. insect bite, ACE-inhibitor use). It is important to explore events leading up to the presentations during the history. This may include:
- Recent illnesses
- New medications (e.g. ACE inhibitors)
- Food ingestion
- Exercise/physical exertion
- Recurrent episodes and family history (?HAE)
- Insect bites/stings
- Travel history
Further investigations depend on the suspected underlying aetiology and severity of the presentation. If an allergic reaction is suspected then patients may be tested for allergen-specific IgE antibodies and referred to immunological for skin prick testing after the acute episode. Often, no underlying cause will be identified in patients with chronic urticaria/angio-oedema.
If isolated angio-oedema is recognised, patients should undergo a basic series of investigations including full blood count, urea & electrolytes, liver function tests, C-reactive protein and complement protein C4. Low levels of C4 should warrant further assessment for hereditary angio-oedema. Many cases of angio-oedema will have normal investigations.
Management
Management of angio-oedema depends on the suspected mechanism, acuity and severity of the swelling.
Angio-oedema with anaphylaxis
Any patient presenting with angioedema as part of a generalised allergic reaction causing anaphylaxis requires urgent management according to the resuscitation council guidance for anaphylaxis. The principal treatment is intramuscular adrenaline. For more information see anaphylaxis notes.
Mast-cell mediated angio-oedema
The principal treatment of mast-cell mediated reactions is with second generation H1-receptor histamine antagonists (e.g. cetirizine, loratadine, fexofenadine). High doses may be required. This follows a similar management strategy to acute urticaria.
Corticosteroids may be used in addition to anti-histamines for severe angio-oedema. This may be given as a one off STAT dose (e.g. 20-40 mg of prednisolone) and then repeated after 24 hours, or it may be given as a short tapering course over 5-7 days.
If angio-oedema is severe or accelerating and patients have (or are at risk of) airway compromise, treatment should be with intramuscular adrenaline similar to anaphylaxis guidelines.
Bradykinin-mediated angio-oedema
The two most common causes of bradykinin-mediated angio-oedema are medications (e.g. ACE inhibitor use) and hereditary angio-oedema. The principal treatments include:
- Medications: stop the drug and monitor for resolution. Rarely therapies used in hereditary angio-oedema may be used
- Hereditary angio-oedema: several pharmacological agents may be used for acute attacks. Some patients require long-term prophylaxis (discussed below).
Importantly, traditional therapies for allergic reactions (e.g. anti-histamines, corticosteroids, adrenaline) have limited efficacy in these bradykinin-mediated angio-oedema.
Regardless of cause, if there is severe airway compromise, patients require urgent airway management by an experienced clinician and will usually be given intramuscular adrenaline similar to anaphylaxis or laryngeal angio-oedema, although efficacy is limited.
Hereditary angio-oedema
Several pharmacological agents are available for the management of acute attacks secondary to HAE. These first-line therapies are given as an intravenous infusion/injection (ex. Icatibant - S/C injection) and can take up to 30 minutes to have an effect.
- Purified C1 inhibitor concentrate: plasma derived or recombinant
- Kallikrein inhibitor (e.g. Ecallantide)
- Bradykinin-receptor antagonist (e.g. Icatibant)
- Fresh frozen plasma (FFP): second line agent. May have a paradoxical effect making angio-oedema worse.
Some patients may require long-term prophylaxis to prevent recurrent attacks. Various options are available (e.g. C1 inhibitor concentrate injections, tranexamic acid, progesterone or androgens).
Recurrent idiopathic angio-oedema
Patients with recurrent angio-oedema may be treated with long-term non-sedating anti-histamines with referral to an immunologist. If attacks are infrequent, patients may be given a single dose of corticosteroid and high dose antihistamine at the onset of the attack.
Last updated: November 2021
Have comments about these notes? Leave us feedback
